Cardiologist Dr Aseem Malhotra says NHS 'system failures' costing 'thousands of deaths yearly'
A leading NHS cardiologist has said that a healthcare "system failure" is resulting in the unnecessary deaths of thousands of patients every year. In comments today (24 February), Dr Aseem Malhotra warned that there is currently an "epidemic of misinformed doctors and misinformed patients in the UK and beyond".
In comments on 23 February in the Mail Online, Dr Malhotra blames biased research funding and reporting in medical journals, as well as commercial conflicts of interest for the "unnecessary deaths". He claimed that public funding is often allocated to medical research only when it is likely to be profitable and not when it would benefit patient care.
Several leading doctors have today supported Dr Malhotra's concerns, calling for the parliamentary Public Accounts Committee to conduct an independent inquiry into the safety of medicines to ensure greater transparency in prescribing drugs to patients. They include the former president of the Royal College of Physicians, Sir Richard Thompson, chair of the BMA General Practitioners committee, Dr Chaand Nagpaul, president of the Faculty of Public Health, as well as the editor in chief of JAMA International Medicine, Rita Redberg.
Expanding on his comments, Dr Malhotra said: "Medical journals and the media can be manipulated to serve not only as marketing vehicles for the industry but be unwittingly complicit in silencing those who call for greater transparency and more independent scrutiny of scientific data."
Citing recent studies, the cardiologist said that prescription drugs are the third most common cause of death after heart disease and cancer. He also noted that the side effects of anti-depressants and dementia drugs are responsible for more than half a million deaths every year in the United States and Europe.
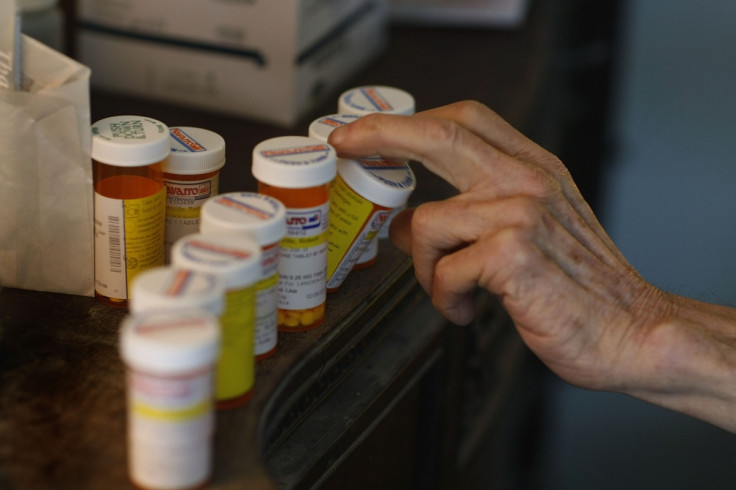
He also said that a "more medicine is better" culture had been created because of financial incentives to prescribe more drugs, stating that those above the age of 75 are particularly vulnerable, with one in three elderly people being admitted to hospital due to an adverse drug reaction.
Supporting Dr Malhotra's comments, Thompson said: "The time has come for a full and open public enquiry into the way evidence of the efficacy of drugs is obtained and revealed. There is real danger that some current drug treatments are much less effective than had previously been thought."
Sir Thompson said that there is a need for closer scrutiny of the evidence underpinning drugs, as well as better promotion of the evidence. He also called for more education of the public, doctors and medical students in how to assess the value of prescribing drugs to different groups of patients.
Dr Malhotra said: "Without full transparency and accountability no doctor can provide what we slogged through medical school and devote our heart and souls to: providing the best quality care for our patients."
© Copyright IBTimes 2024. All rights reserved.






