Muscle From Skin Cells to Fix Damaged Hearts
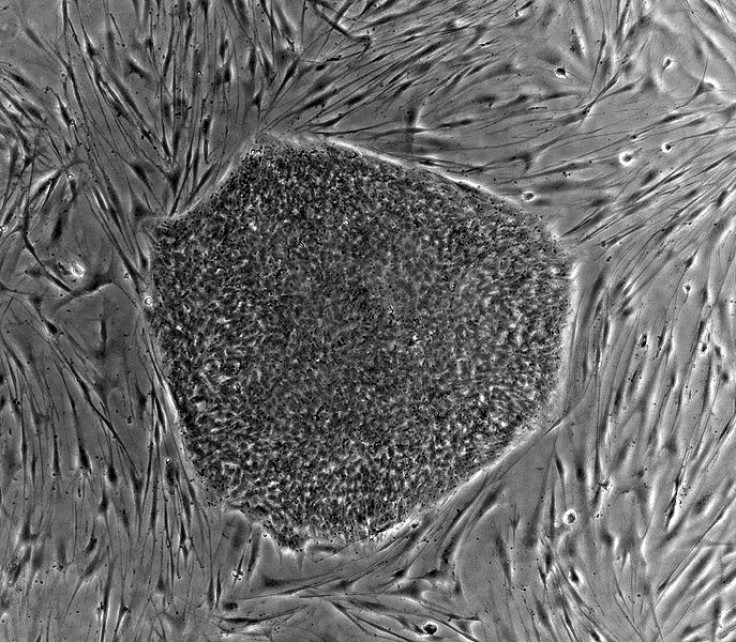
Scientists from the Technion-Israel Institute of Technology have found a way to use a patient's skin cells and convert them into heart muscle to repair damaged heart. They claim that the method is very effective compared to a previous technique. In this method the stem cells, also known as human induced pluripotent stem cells (hiPSCs), are taken from the patient's body itself, so the patient's immune systems does not reject the cells as "foreign bodies".
"What is new and exciting about our research is that we have shown that it's possible to take skin cells from an elderly patient with advanced heart failure and end up with his own beating cells in a laboratory dish that are healthy and young - the equivalent to the stage of his heart cells when he was just born," said Professor Lior Gepstein, Professor of Medicine (Cardiology) and Physiology at the Sohnis Research Laboratory for Cardiac Electrophysiology and Regenerative Medicine, Technion-Israel Institute of Technology .
Recent advances in stem cell biology and tissue engineering have enabled researchers to consider ways of restoring and repairing damaged heart muscle with new cells, but a major problem has been the lack of good sources of human heart muscle cells and the problem of rejection by the immune system.
Recent studies have shown that it is possible to derive hiPSCs from young and healthy people and that these are capable of transforming into heart cells. However, it has not been shown that hiPSCs could be obtained from elderly and diseased patients. Now researchers are able to create heart muscles with the patient's stem cell.
Scientists had conducted a study on two heart patients aged between 51 and 61. The team took skin cells from two men with heart failure and mixed the cells up with a cocktail of genes and chemicals in the lab to create the stem cell treatment, according to a BBC report.
This stem cell was then transplanted into the patients' hearts and they found that this method was very effective because the patients' immune system did not reject the cells.
"In this study we have shown for the first time that it's possible to establish hiPSCs from heart failure patients - who represent the target patient population for future cell therapy strategies using these cells - and coax them to differentiate into heart muscle cells that can integrate with host cardiac tissue," said Prof Gepstein.
Scientists will be carrying out further research into some of these areas, including evaluating using hiPSCs in cell therapy and tissue engineering strategies for repairing damaged hearts in various animal models, investigating inherited cardiac disorders, and drug development and testing.
© Copyright IBTimes 2024. All rights reserved.