Gonorrhoea treatment appears to speed the spread of antibiotic resistance
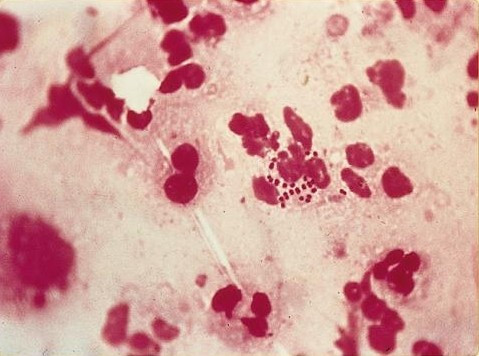
High rates of treatment of gonorrohea appears to be speeding up antibiotic resistance. In a catch-22 scenario, scientists discovered that treating the sexually transmitted infection increases resistance to the last remaining antibiotic used to treat it.
Sexually transmitted bacteria Neisseria gonorrhoeae has developed a resistance to most antibiotics, limiting possibilities of treatment for infected individuals. The study, published in PLOS Pathogens looked at what drives resistance spread in two different host populations; heterosexual men and men who have sex with men (MSM).
The authors used these information to anticipate future resistance trends and improve antibiotic treatment strategies.
First-line treatment
Today, ceftriaxone is the one last antibiotic remaining recommended as first-line treatment, because most strains of the Neisseria gonorrhoeae bacteria are now commonly resistant to other antibiotics, like penicillin or fluoroquinolones.
However, scientists now worry that the sole use of ceftriaxone to treat gonorrhoeae is also progressively spreading resistance against this antibiotic.
"The problem we have is that today we typically treat gonorrhoea with only one type of antibiotic. Taking into account the pathogens evolution, a diversified treatment might be a better strategy" one of the authors, Christian Althaus from the University of Bern, told IBTimes UK.
The scientists looked at data collected in two surveillance projects in the UK and the US, and constructed a mathematical model to describe rates of resistance spread based on people's sexual behaviours and prevalence of infections. They were able to determine the speed at which resistant strains are transmitted among heterosexual men, and men who have sex with men.
Not the number of partners
Resistance appears to spread quicker in MSM, with an estimated bacteria doubling time of 6 months compared with 16 months in heterosexual men. The scientists intuitively thought this was because these men traditionally have more sexual partners and were therefore more likely to be infected - including with resistant strains.
Yet their model indicated otherwise. Rather than a higher number of partners, it was a higher level of antibiotic treatment for infections among MSM that was responsible for the faster spread of resistance. The researchers thus believe treatment rate is the main driving force of resistance spread.
Developing new testing methods
This has implications for how patients should be treated."Treating too much leads to increased resistance but we can't stop treating people either. The alternatives are developing better testing methods to rapidly detect with what strains of gonorrhoeae a person is infected with and whether they are resistant or susceptible to certain types of antibiotics", says Althaus.
"Until then, the level of gonorrhoea that is resistant to first-line treatment should be closely followed and alternative treatment options should be considered."
Unlike what is recommended today, it is possible to treat certain strains of gonorrhoea with antibiotics that were already used ten or twenty years ago. But for that, physicians would need to know exactly with what strains the person is infected with, and to which antibiotics they are resistant. That's why new testing methods are needed.
© Copyright IBTimes 2025. All rights reserved.






















