Treatment for Alzheimer's a step closer as trial shows promising results in reducing amyloid plaques
The drug targets amyloid plaques in the brain, a hallmark of the disease.

An antibody therapy designed to reduce the build-up of amyloid plaques in the brains of patients with mild Alzheimer's disease has shown promising results in early clinical trials. The treatment also appears to be safe, with relatively few side effects.
It has been 25 years since deposits of the amyloid-β (Aβ) protein in the brain have been identified as a hallmark of the disease. A consensual theory is that Aβ-related toxicity is the primary cause of synaptic dysfunction and neurodegeneration associated with the disease. Several anti-Aβ treatments have been tested in the past to target the protein, but they have had limited success.
This latest study, published in the journal Nature, reports on the results of a 12-month placebo controlled trial of an antibody known as "aducanumab". It suggests this drug has a real potential in reducing the accumulation of amyloid plaques in the brains of people suffering from an early, mild form of Alzheimer's.
The antibody may also have clinical benefits, as the scientists found evidence of slowing-down of cognitive decline, although more studies need to be conducted to verify this.
Transgenic mice and Alzheimer's patient
Aducanumab is a human monoclonal antibody that selectively targets aggregated Aβ. This means that it is derived from humans' immune B-cells, and reacts with different types of Aβ aggregates, such as soluble oligomers and insoluble fibrils.
In preclinical trials with transgenic mice, the international team of scientists (Switzerland and US) showed that a drug similar to aducanumab drastically reduced amyloid plaque build-up. They discovered that the antibody was capable of crossing the blood–brain barrier, engaging its target, and clearing Aβ from the mice's brains.
These positive results prompted the launch of clinical trials in humans. A total of 165 patients in the early stages of the disease, with mild clinical decline, were recruited. They received either monthly intravenous infusions of aducanumab – at different doses for different groups – or a placebo.
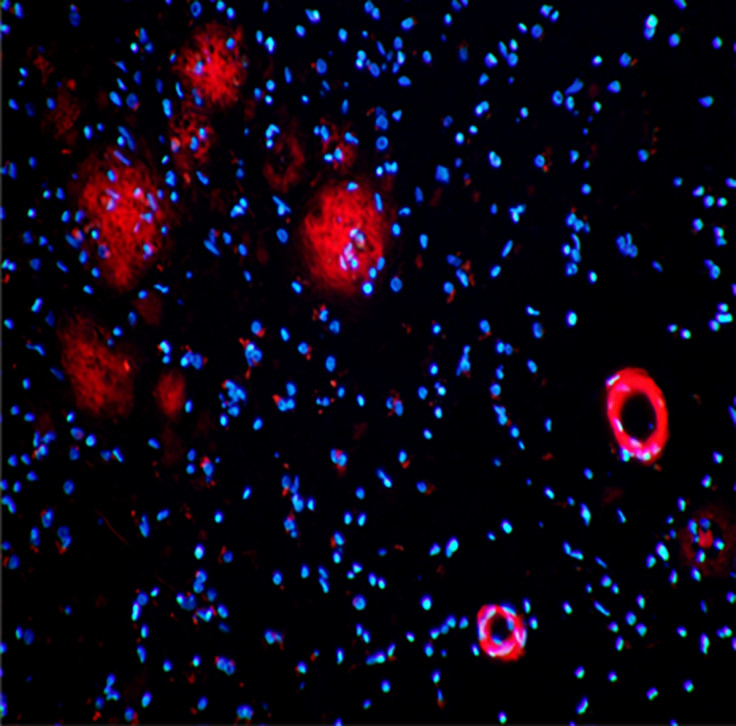
Over the course of the study, the scientists observed on PET scans dose-dependant improvements in the brains of patients receiving the antibody. The greatest doses given were associated with greater reductions of Aβ plaques. In contrast, very little changes were witnessed on the scans of participants who had received the placebo.
The findings have been welcomed with cautious optimism in the scientific community. "The degree of reduction of amyloid aggregates in the brain of people who received the treatment is fairly unprecedented. This is perhaps the best news we have had in my 25 years working on Alzheimer's disease," Dr Stephen Salloway from Brown University, one of the study's authors, said during a press conference.
However, experts agree that this will have to be confirmed in larger clinical studies with much bigger samples of participants. "This was not a phase three study. It was not powered or designed to identify treatment effects, and, even in the context of apparently positive data, we need to consider the possibility of selective subject drop out and chance as underlying the positive findings. These new data are tantalising, but they are not yet definitive", said John Hardy, professor of neuroscience at UCL.
Side effects to monitor
The main objective of this trial was to test the safety and tolerability of the drug. Over the course of the trial, 40 participants abandoned the study – half of them were people who had experienced side effects from the treatment. The issue they encountered is known as amyloid-related imaging abnormalities or ARIA – abnormalities in the brain observed by MRI scans, which are generally asymptomatic. Treatment was discontinued if the changes in the brain appeared particularly severe – suggesting a slightly higher risk of hemorrhages – or if people experienced symptoms such as headaches or confusion.
No one was hospitalised and these adverse events were dose and genotype dependant, meaning individuals who were most affected were ones receiving the higher doses or those with a specific genetic mutation.
As phase three trials for aducanumab begin, scientists say they will dose the drug a bit differently for these individuals to make sure they can benefit from it without endangering their health. "Because ARIA happens relatively early in treatment, the hope is it could be addressed by adapting the doses quickly and introducing them more gradually," Salloway explained.
A cognitive decline?
Although assessing the drug's effects on clinical symptoms of Alzheimer's disease was not the goal of this study, the authors conducted an exploratory investigation with the participants to assess whether the antibody could potentially prevent cognitive decline.
With different tests looking at cognitive function and daily functioning, they uncovered hints of cognitive benefits for people who received the treatment, with the greatest effects for those on the higher doses. "During the first six months of the trial, all groups saw their cognitive decline worsen, as is expected in this disease, but after week 26, people who were given the the drug stayed stable in their cognitive function while those on placebo worsened significantly", Salloway pointed out.
The impact of the drug on cognitive function will now be investigated in greater depth, with hopes that the condition of people with the disease may eventually stop deteriorating. "As we await the results of our trials and other studies, the hope is that patients will get access to a range of suitable new treatments in future years, some of them efficiently targeting amyloid plaques," concluded another study author, Alfred Sandrock, from biotechnology company Biogen.
The study was led by scientists from pharmaceutical companies Biogen and Neurimmune (Zurich).
© Copyright IBTimes 2025. All rights reserved.




















