Designer immune cells cure baby of blood cancer in landmark case
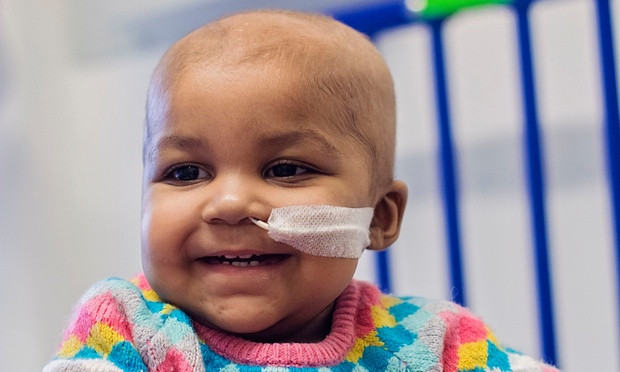
In a first of its kind therapy a baby with aggressive leukaemia has been cured of cancer. This was possible with the help of genetically engineered immune cells that were able to kill the drug resistant cancer cells.
One-year-old Layla Richards was treated by specialists at Great Ormond Street Hospital in London, using a method not tested on humans so far. It was used after Layla was given a few months to live following the failure of conventional treatment.
After the first infusion of the modified cells, Layla remained clear of leukaemia and two months later, doctors gave her a second bone marrow transplant to replace her entire blood and immune system. She is now fully cured and was at home.
Professor Waseem Qasim, professor of Cell and Gene Therapy at UCL ICH and Consultant Immunologist at the hospital, explained: "We have only used this treatment on one very strong little girl, and we have to be cautious about claiming this will be a suitable treatment option for all children."
"But this is a landmark in the use of new gene engineering technology and the effects for this child have been staggering," he said.
The designer cells were donated T cells, or white blood cells, which were modified to carry an extra gene to target leukaemia cells. They also had to have some genes disabled to stop them from attacking patients and render them invisible to drugs used to suppress patients' immune systems. Using molecular tools (Talen®) that work like scissors snipping genes, the T-cells were engineered.
"The approach was looking incredibly successful in laboratory studies, and so when I heard there were no options left for treating this child's disease, I thought 'why don't we use the new UCART19 cells?" Qasim said.
When Layla was three months old, she was diagnosed with infant acute lymphoblastic leukaemia. It was one of the most aggressive cases that doctors had seen.
Chemotherapy and bone marrow transplant to replace her damaged blood cells did not help. It was then that doctors had given up and suggested palliative care, but the child's parents asked the doctors to keep trying.
After approval from the ethics panel, researchers at UCL went ahead with the infusion of cells tried successfully on mice with leukaemia. The results expected whether the cells were working appeared after two weeks and Layla was clear of the disease.
Full clinical trials funded by Cellectis are now being planned to test Ucart19 cells in larger groups of patients and are set to begin early in 2016.
"Cellectis main objective is to provide cancer patients with an accessible, cost-effective, off-the-shelf allogeneic CAR-T therapies across all geographies. With clinical trial for the first gene-edited UCART on the horizon, it could be the beginning of a revolution in cancer immunotherapy," said Dr André Choulika, chairman and CEO of Cellectis.
© Copyright IBTimes 2025. All rights reserved.



















