India: Poorly educated rural health providers wreaking havoc on child health
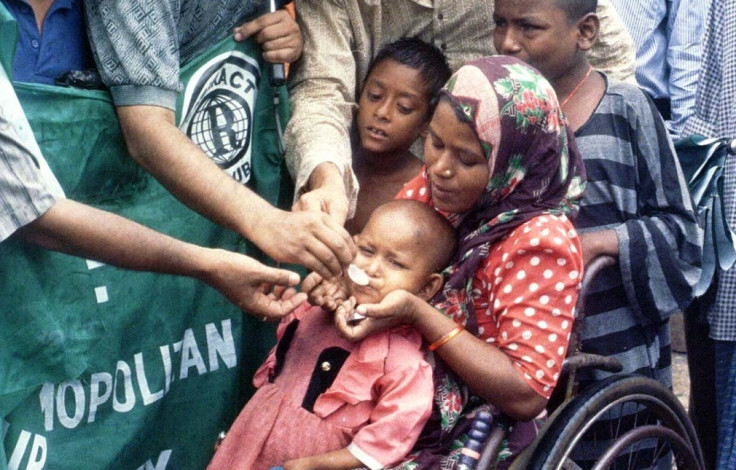
Unnecessary antibiotics and harmful drugs are causing much damage among children in rural India, says a Duke University study. This has been linked to poor levels of medical training and knowledge among health providers.
Diarrhoea and pneumonia accounted for 24% of deaths among children one to four years old, with approximately two million deaths worldwide in 2011.
Bihar in India where the study was conducted has an infant mortality rate of 55 per 1,000 live births, the highest in the country.
Instead of prescribing lifesaving treatments such as oral rehydration salts (ORS), the medical practitioners prescribe unwanted antibiotics or other potentially harmful drugs, says Manoj Mohanan, a professor in Duke's Sanford School of Public Policy, and lead author of the study.
The study involved 340 health care providers who were tested for their diagnosis and treatment methods. Later, individuals who portrayed patients presenting the same symptoms as in the interviews made unannounced visits.
This enabled researchers to measure the gap between what providers know and what they actually do - the "know-do" gap.
Providers exhibited low levels of knowledge during the interviews and fared worse during the practice.
For example, for diarrhoea, while 72% said they would prescribe oral rehydration salts, only 17% actually did so. Those who did prescribe ORS added other unnecessary or harmful drugs.
In practice, none gave the correct treatment: only ORS, with or without zinc, and no other potentially harmful drugs.
Almost 72% of providers gave antibiotics or potentially harmful treatments without ORS.
"Massive over-prescription of antibiotics is a major contributor to rising antibiotic resistance worldwide," Mohanan says. "Our ongoing studies aim to understand why providers who know they shouldn't be prescribing antibiotics for conditions like simple diarrhoea continue to do so."
He clarifies that it was not demand from patients that resulted in antibiotics prescription, as most patients in the study did not ask for it.
India has emerged as the world's largest consumer of antibiotics with a 62% increase in use over the last decade, according to a Princeton University study.
India's antibiotic use went up from eight billion units in 2001 to 12.9 billion units in 2010.
Self-medication
In fact, indiscriminate antibiotic use and self-medication in India have seen cases of bacteria resistant to colistin, the last available drug in the world.
"The Know-Do Gap in Quality of Health Care for Childhood Diarrhea and Pneumonia in Rural India" is published online by JAMA Pediatrics.
Health providers in rural settings have little medical training and very little knowledge of how to treat the two common and deadly ailments. Most have no medical degree.
Even providers with formal medical training exhibited large gaps between what they knew and did, but at least were less likely to prescribe harmful medical treatments.
"Our results show that in order to reduce child mortality, we need new strategies to improve diagnosis and treatment of these key childhood illnesses," Mohanan says.
"Our evidence on the gap between knowledge and practice suggests that training alone will be insufficient. We need to understand what incentives cause providers to diverge from proper diagnosis and treatment."
© Copyright IBTimes 2025. All rights reserved.



















