Sleeping sickness parasites found to hide under the skin – paving way for new diagnosis tool
The discovery suggests scientists may not have to rely simply on blood tests to diagnose sleeping sickness.
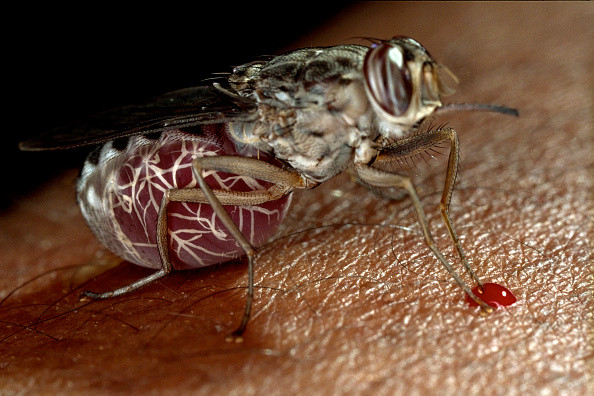
The parasites that spread sleeping sickness have been shown to stay under the skin of infected patients, not just in their blood, scientists have found out. This discovery could transform the way the disease is diagnosed, and influence how quickly it can be treated.
Sleeping sickness is prevalent in 36 sub-Saharan countries where tsetse flies – the primary transmitters of the disease – are often found. Just under 10,000 people have been diagnosed with the illness annually in recent years, by analysing blood samples for the presence of the Trypanosoma brucei gambiense parasite which is responsible for 98% of all cases (see box).
However, scientists have in the past identified cases of infections in which parasites remained undetected or were identified only in low concentrations in the blood.
They therefore hypothesised the existence of another anatomic reservoir of infection in the body – the skin.
Parasites hiding under the skin
To conduct the research, published in E-life, the scientists used mice and infected them with the sleeping sickness parasite, which they had genetically modified to be fluorescent – and therefore traceable in the bodies of the rodents. The researchers then tracked the dispersion of parasites in the mice after infection, and found that it was more present in the skin than in the blood.
Following this first experiment, they carried out tests in humans. They analysed human skin biopsies, where they identified parasites, even in samples of individuals who had previously not been diagnosed with blood tests. The scientists thus concluded that skin, both in animals and humans, represents a reservoir for the infection – one where the parasites hide.
This may have consequences for how the disease is diagnosed and subsequently treated in the future. "The identification of this novel reservoir requires a re-evaluation of current diagnostic methods and control policies," the authors write. Coming up with new tools that quickly identify Trypanosoma brucei gambiense under the skin, and testing both at the blood and the skin of people suspected to be sick may become crucial steps to fight off sleeping sickness.
What is sleeping sickness?
Sleeping sickness, also known as trypanosomiasis, is a disease transmitted to humans and animals primarily by the tsetse fly. It is endemic in 36 sub-Saharan countries, where the insect is present. The fly is found in other countries, but for some unknown reason, the disease only strikes in Sub-Saharan Africa.
Trypanosomiasis is a parasitic disease – in this case, protozoan parasites belonging to the genus Trypanosoma are responsible with 98% of cases blamed on Trypanosoma brucei gambiense.
The strange name given to the disease is due to one of its most important symptoms – a disturbance of the sleep cycle. This, along with most other symptoms, appear late in the disease, during what is known as the neurological or meningo-encephalic stage. Neurological problems, changes of behaviour, confusion, sensory disturbances and poor coordination are frequently observed.
Before that, patients may have experienced fever, headaches, joint pains and itching during a first phase known as the haemolymphatic stage. If left untreated, the condition can be fatal.
While the number of cases is now below 10,000 annually, the estimated population at risk is 65 million people. Diagnosis includes screening for potential infection with blood tests and clinical signs like swollen cervical lymph nodes, establishing if the parasite is present in body fluids and finally determining the stage of the disease.
How it is treated depends on the stage of the disease. Drugs used in the first stage are safer and easier to administer than those for second stage, and the sooner the diagnosis is done, the easier it is to cure sleeping sickness. The problem is that the disease can be confused with many others in its first stage so it is often hard to diagnose early.
In the second stage of the disease, treatment success depends on drugs that cross the blood-brain barrier to reach the parasites - such drugs are particularly toxic and complex to administer.
© Copyright IBTimes 2025. All rights reserved.





















