World Meningitis Day 2016: 24 hours can mean the difference between life and death
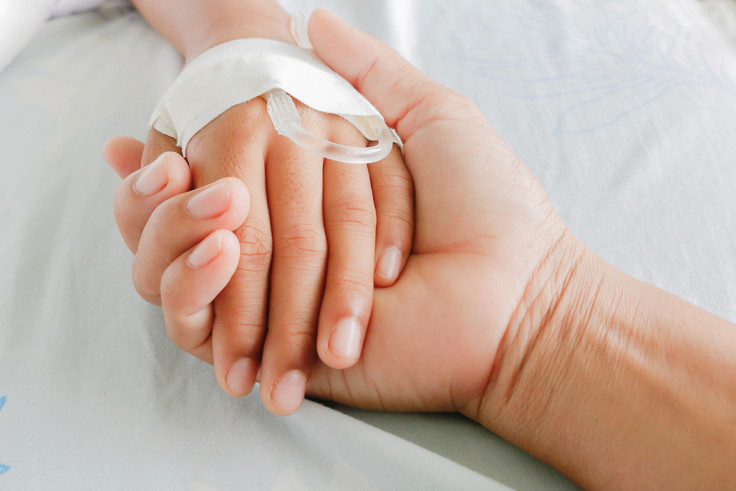
In November 1982, Steve Dayman lost his infant son Spencer to meningitis B and septicaemia. He still remembers the phone call his wife made him that autumn afternoon, telling him that their little boy was not his usual self. Just 24 hours after being admitted into hospital, Spencer's body could not fight the disease any longer, and his breathing stopped.
In memory of his son, Dayman has spent the last three decades raising awareness about bacterial meningitis, converting his personal struggle against the disease into a major public health issue. He is the executive founder of charity Meningitis Now. As years have gone by, he has witnessed a lot of positive changes. "In 1982, there were no charities to help families like us. We have come a long way since then, and received a lot of support" he recalls.
Diagnosing meningitis
Dayman has seen preventative efforts increase over the years, with a big step forward coming when World Meningitis Day was created in 2009 by the Confederation of Meningitis Organsations (CoMO). Taking place annually on 24 April, this year's focus will look at alerting families about how quickly the disease can spread, with the motto "24 hours! Time to act".
Families who have lost a loved-one to meningitis will recognise the motto well: twenty-four hours can make the difference between life and death in meningitis cases. The disease can progress very rapidly, going from what looks like a viral infection to a more severe illness in the space of just a few hours.
Though World Meningitis Day has been effective in raising the global profile of meningitis, parents and healthcare workers sometime still struggle to diagnose the disease.
"If your child has meningitis, you will notice a quick deterioration in just a few hours. In the case of Spencer, he looked healthy in the morning, but after his mid-day nap he was not his usual self, calling out for us to get him out of the bed", Dayman told IBTimes UK. "The problem is that there is not a set pattern for the disease to develop. Often, parents know about the rash associated with septicaemia, but this can be a very late symptom of the disease".
Hospital paediatrician Catherine Weil-Olivier says the diagnosis is relatively easy to make for children who are older than two or three - but the problem is early diagnosis for babies and teenagers. "During adolescence, the symptoms of bacterial meningitis can be mistaken with that of other diseases. The disease is often mistaken for the flu. This makes it difficult for parents to react at the right moment", she says.
So what should parents do? "In the end, parents know their children best, they do not call emergency services unless they are really concerned. They should not be frightened to tell health services 'I want you to consider meningitis'", Dayman says.
Vaccination campaigns in the UK
Over the last twenty years, vaccines have also radically changed the nature of the fight against the disease." Most experts say treatments cannot be improved, leaving us with one solution, vaccination. Vaccines have been the milestones in the fight against meningitis.", Dayman points out.
In 1992, the first vaccine to be introduced, against Haemophilus influenzae type B, led to this type of infection completely disappearing. Seven years later, in 1999, the vaccine against meningitis C further stopped the spread of infections.
Implemented in 2006 in the UK, the routine vaccination programme against pneumococcal infections, recommended for infants and toddlers, was another step forward, especially for older adults who are more vulnerable to pneumococcal meningitis, and who were thus protected indirectly.
This conjugate vaccine has offered good protection against the serotypes included in the vaccine (initially 7 then 13 from 2010), but it will need some improvement adaptation to the ongoing epidemiology in the coming years."This vaccine now targets the thirteen most predominant types of pneumococcus, but new other serotypes are emerging, meaning we will need to re-think these vaccines. Researchers currently investigate this issue", explains Catherine Weil-Olivier.
The most recent - and, perhaps, most ground-breaking discovery - was the meningitis B vaccine, in 2014. MenB has traditionally been the most common bacterial strain in the UK, especially for children under the age of one.
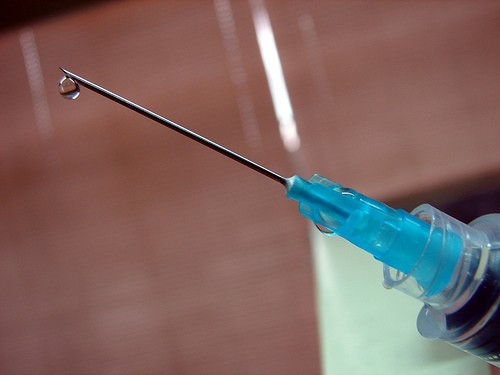
Recommended for babies aged eight weeks (followed by a second dose at 16 weeks, and a booster at one year), it is one of the country's greatest vaccination success' in recent years. "This does not mean we should stop there. Currently the meningitis B vaccine only protects against 88% of B meningococcus bacteria, and we need to improve this", Dayman nuances.
Finally, the meningitis ACWY vaccine also offers protection against four types of bacteria that can cause meningitis – meningococcal groups A, C, W and Y. Young teenagers and students, going to university for the first time, are encouraged to have it - but according to Dayman, they are the hardest age group to convince of the benefits of vaccination. Targeted prevention campaigns are therefore crucial.
"Pursuing the efforts to make sure as much people as possible are aware of the symptoms and the risks, as well as improving and promoting vaccines has made a huge change. We have seen very positive evolutions in the past 30 years. I am convinced that in 30 years time, meningitis will be confined to textbooks", he concludes.
© Copyright IBTimes 2025. All rights reserved.





















