Britons could face delay in getting access to new drugs after £20m a year cap put in place
New measure could delay new drugs being made available on NHS by as long as 3 years.
The NHS cost watchdog has imposed a £20m-a-year cap on the cost of new drugs to be introduced in the National Health Service in England in a move to ease the financial pressure faced by the healthcare provider.
The new measure could lead to delays of up to three years before new drugs are available on the NHS. The measure is aimed at giving NHS chiefs the opportunity to re-negotiate drug prices with pharmaceutical companies.
Under the current system, drugs that are assessed as cost-effective by the National Institute for Health and Care Excellence (Nice) are automatically recommended for use in the NHS and the health service has 90 days to start offering them to patients.
The present system looks only at the cost versus the benefits of the drug on the basis of the impact on an individual. It does not consider how many people may take the drug and therefore the total cost to the system, the BBC notes.
The new measure, which was agreed by Nice, will be introduced from April after a public consultation launched in October 2016. The new policy will be reviewed in three years to assess its impact.
According to the BBC, patient groups and the drug industry have already objected to the plan.
The new changes include:
- Fast track option for appraising treatments which offer exceptional value for money. The target is for these drugs to be available to patients a month after they are licensed
- Budget impact test where drugs costing more than £20m in any one of their first three years of use will trigger commercial discussions between the pharma company and the NHS England to mitigate the impact on the rest of the NHS.
- If a deal cannot be reached to reduce costs on these drugs, NHS England can seek an extended period to introduce the drug in a phased manner - usually for no more than three years.
- Drugs for very rare diseases will now be evaluated against a sliding scale - the more the medicine costs, the greater the health benefit it must offer to be approved for routine NHS use by NICE.
"We believe these and other changes that have now been approved will enhance our ability to optimise access to innovative treatments in the light of the significant financial challenge facing the NHS," the watchdog's chief executive, Sir Andrew Dillon, said in a statement.
"We are taking forward the proposal for more flexibility in the adoption of technologies into the NHS which are cost effective but which have a predicted budget impact of £20m or more during the first 3 years. Companies will have the opportunity of confidential negotiations with NHS England, to help avoid and minimise delays in patients having access to treatments recommended by Nice.
"We believe these and the other changes that have now been approved will enhace our ability to optimise access to innovative treatments in the light of the significant financial challenge facing the NHS," Dillon said.
Fast track appraisals
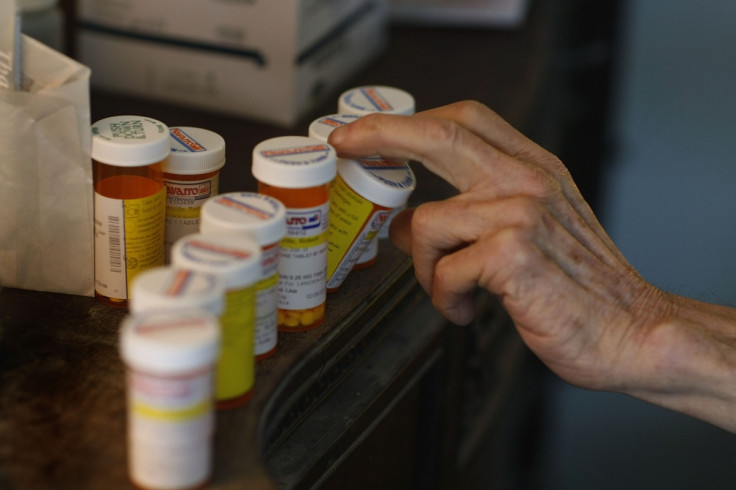
Nice said the fast track appraisals will apply to drugs with a likely cost-per-extra-year of quality-adjusted life (QALY) of under £10,000. The upper end of Nice's standard threshold range is £20,000 - £30,000 per QALY.
The watchdog has also signalled its intention to consider widening the fast-track approach to a wider group of treatments, to cover medical devices and diagnostics over the next two years.
Rare disease treatments
Nice also said that it is introducing greater flexibility on how it evaluates treatment for very rare conditions under its Highly Specialised Technologies programme. It is raising the upper limit by 10 times the standard NICE threshold to reflect the transformational health benefits it can offer.
Treatments deemed to provide significant QALY benefits could be assessed against a maximum threshold of £300,000 per QALY rathern than the £100,000 QALY limit that was in the original proposal, the Nice statement added.
NHS England's Acting Director for Specialised Commissioning, John Stewart, said: "These are not easy decisions, but we are committed to working closely with companies that are willing to price their products responsibly and this new flexibility will help us develop innovative win/win/win agreements - good for patients, good for taxpayers and good for those companies that are willing to price responsibly."
In 2016, the NHS spent £16.8bn on drugs, up from £13bn on 2011. The BBC says there is concern that a breakthrough in areas like dementia could potentially cost the NHS billions of pounds.
© Copyright IBTimes 2025. All rights reserved.