India: Over 200 swine flu deaths in less than two months raising concerns
Around 215 deaths from swine flu have been reported so far this year across India, in contrast to 238 deaths in 2014 raising fears of an epidemic.
Hundreds more have tested positive in these states.
There is also a rise in mortality rate seen this time with deterioration in infected people being swift and patients dying within two days of reporting the case.
Doctors treating patients say that anti-viral drugs such as Tamiflu and Oseltamivir seem to have no effect.
With 81 deaths in Rajasthan, 71 in Gujarat, 30 in Telangana, six in Karnataka and a few deaths from Maharashtra and Haryana, the air-borne virus looks set to cause more damage.
Symptoms and treatment
The symptoms are the same as the seasonal flu -- cough, sore throat, and body aches. Young children, pregnant women, and older adults are more likely to develop complications.
An attack of swine flu may come with nausea, stomach cramps and diarrhoea. In up to half of all cases seen, people never develop a fever.
Shortness of breath, chest pain or blue lips are seen in the severe form of the flu. People with these symptoms should start on an antiviral at once even if symptoms have started since two days, say experts.
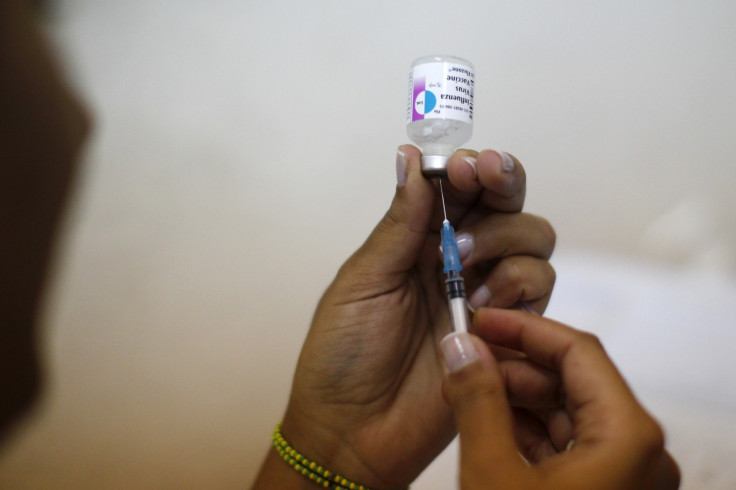
Tamiflu and Relenza are the drugs commonly used to treat or prevent swine flu. But an annual flu vaccine is the best bet against this virus, according to WebMD.
The WHO and the Indian Academy of Paediatrics (IAP) have recommended trivalent influenza vaccine be administered to high-risk groups. Vaccines available in the market are manufactured and sold by different companies with the cost of one shot ranging between Rs 700-800.
Most of them are imported.
Mode of spreading
The virus spreads through air and contact like any other flu virus. Besides inhaling air borne pathogens, touching an infected surface can spread the virus. An infected person can be contagious for up to 10 days.
Swine flu is spread by large air droplets and wearing a face mask could protect against inhaling the droplets, though its efficacy hasn't been tested. However, during the 2009 outbreak, Canadian nurses wearing an N95 mask, which keeps out most viral particles got flu just as often as they did wearing a cloth mask.
Frequent hand washing and avoiding hand contact with eyes, nose or mouth are believed to be the best ways to avoid infection.
But just as with the mask, there is not much hard evidence that hand-washing works except perhaps among young children.
What may work is keeping the body fit with exercise. A study in mice back then had found just a single session of exercise before catching flu reduced disease severity, while regular exercise beforehand worked even better.
Swine flu, also known as 2009 H1N1 type A influenza, is a human disease. People get the disease from other people, not from pigs.
It originally jumped to humans from pigs in which it evolved. The virus is a "reassortant" -- a mix of genes from swine, bird, and human flu viruses.
The H1N1 influenza virus was first detected in 2009 when it spread rapidly around the globe after it was first identified in Mexico. The US Centers for Disease Control (CDC) estimates that the global death toll from the 2009 pandemic was more than 284,000. In the US alone it killed 12,500.
The World Health Organization declared the outbreak the first worldwide pandemic in more than 40 years.
Evolving virus
The 2009 H1N1 virus was very different from previously circulating human H1N1 viruses and, therefore, vaccines available at that time did not provide protection against 2009 H1N1 viruses.
However, the virus is now commonly spread in people and the current seasonal flu vaccines are believed to provide protection against these viruses.
Most swine influenza viruses (SIVs) do not cause disease in humans. However, the H1N1 virus that caused the influenza pandemic in 2009-2010, thought to have originated in swine, is an example of an SIV that spread easily among people and also caused disease, according to WHO.
Pigs can become infected with influenza viruses from a variety of different hosts (such as birds and humans), and act as a "mixing vessel," facilitating the reassortment of influenza genes from different viruses and creating a "new" influenza virus.
Such "new" reassortant viruses may be more easily spread from person to person, or may cause more severe disease in humans than the original viruses.
The primary risk factor for human infection appears to be direct or indirect exposure to infected live or dead animals or contaminated environments.
Virus mix
During the 2009 pandemic, the H1N1 virus crowded out other influenza viruses to become the dominant virus. This is no longer the case as many countries are reporting a mix of influenza viruses.
According to the WHO's International Group on Strategy and Management of Zoonotic and Public Health Risks at Human-Animal Interface, from the second half of 2009 till the first quarter of 2011, A (H1N1) was the predominant influenza virus in India.
While the second half of 2011 showed lower activity of this strain and A (H3N2) and B group viruses dominated, again from the beginning of 2012 the pandemic strain of A (H1N1) has reappeared and co-circulated with group B and A (H3N2) viruses.
Recently, published studies indicate that 20–40% of populations in some parts of the world have been infected by the H1N1 virus and thus have some level of protective immunity.
Many countries have good vaccination coverage, especially in high-risk groups, and this coverage further increases community-wide immunity.
Global warming is seeing a rise in disease transmitting insects and pathogens. Loss of biodiversity of species in ecosystems is also spurring the rise in pathogens.
Wetland degradation for instance is being cited as one of the reasons for bird flu cases in India. Loss of its habitat forces the migrating waterfowl that harbour avian influenzas into sites where they have contact with domestic fowl.
The risks of novel and emerging infectious diseases are much higher today with studies showing a quadrupling of disease emergence in the past 50 years.
Around 60% of the diseases spread from animals to humans with a majority traced to wild animals.
© Copyright IBTimes 2025. All rights reserved.




















