Doctors Renew Calls for Opt-Out System for Organ Donation
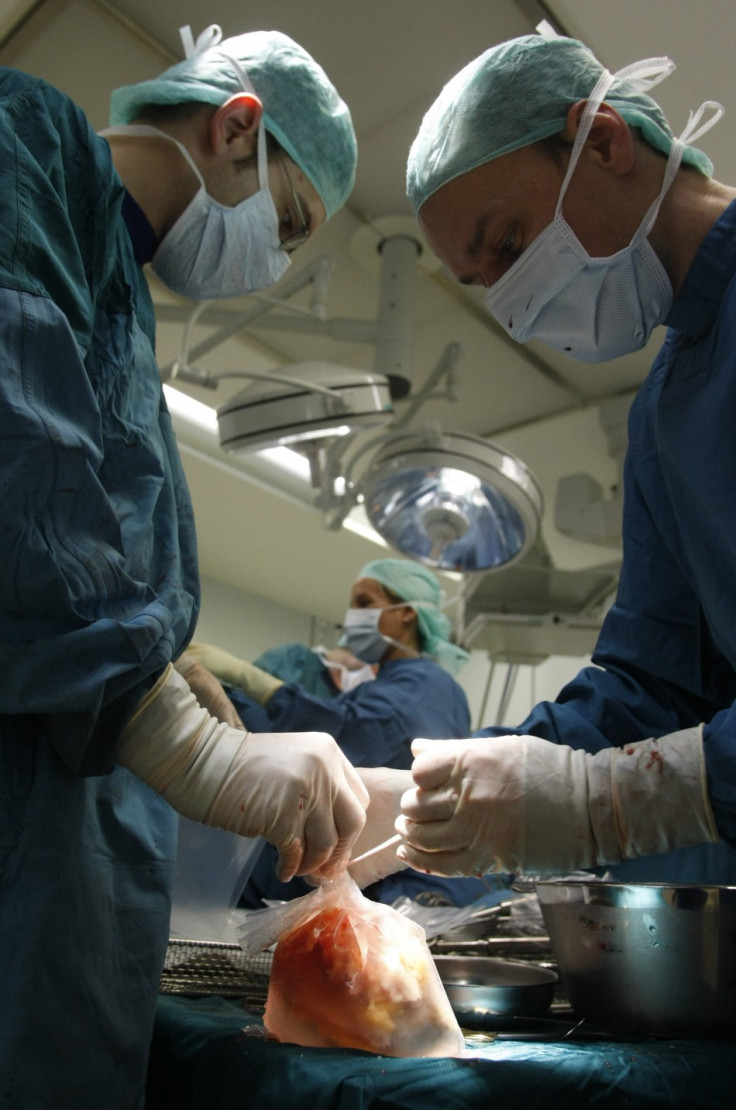
The British Medical Association claims that a major shakeup of public policy on organ donation is needed to stop hundreds of patients dying on waiting lists.
The report concludes that even if the number of donors were increased by 50 percent by 2013, as recommended by the Organ Donation Taskforce, people will still die unnecessarily.
Titled Building on Progress: Where Next for Organ Donation Policy in the UK? the report concludes that a public debate is needed to consider options for increasing donor numbers.
It suggests new approaches including controversial elective ventilation, the use of organs from "higher-risk groups" such as older people, and paying the funeral expenses of those who donate.
"We are at a crossroads in terms of public policy. As a society we need to decide whether we should accept that we have done all we can or whether we should move forward, cautiously and look at other options for increasing the number of donors," said Dr Tony Calland, chairman of the BMA's medical ethics committee.
"There needs to be a public debate on what will work for the UK so that people on the transplant list do not die waiting for a donor.
"These are complex issues that throw up many ethical challenges. It is important that society discusses them openly in a reassuring way. The aim here is to save lives while at the same time protecting individual rights and autonomy.
"While our report explores a number of options the BMA continues to believe that an opt-out system with safeguards is the best way forward for the UK."
The Question of Presumed Consent
Under an opt-out system everyone would be assumed to donate their organs after their death, unless they elected to remove themselves from the donor list.
Safeguards would be put in place, such as family members being consulted as to a person's wishes even if they had not formerly opted out.
"Those who oppose such schemes suggest that the decision is being taken out of the hands of the individuals and the government is taking and using organs without consent," the report states.
"Individuals, and their families, are thus denied the right to make a personal decision and so their autonomy is undermined. It is important to recognise, however, that under an opt-out system individuals have exactly the same decision to make - to donate or not to donate - and so the decision clearly still rests with the individual."
Can Public Policy Maintain Balance With Personal Autonomy?
Other options considered include elective ventilation, a controversial practice that starts ventilation on a patient who is considered close to death with the "specific intention of facilitating organ donation".
Currently, artificial ventilation is continued only for the patient's family to be given the chance to say goodbye or for arrangements to be made for authorised organ removal.
Organ donation in the UK is governed by the Human Tissue Act 2004 and the Human tissue (Scotland) Act 2006. Under this legislation, any procedure or intervention must be in a patient's best interest.
Elective ventialtion was intrioduced in Exeter in 1988, leading to a 50 percent increase in the number of organs suitable for donation. However, it was deemed an unlawful practice by the Department of Health and dropped in 1994.
"Elective ventilation is not an easy option but it has been shown to increase donation rates and to facilitate the wishes of a group of patients who want to donate and would otherwise be unable to do so," the report states.
"The BMA is not calling for the law to be changed to permit elective ventilation, but believes this may be an issue that would benefit from debate both to assess the clinical, legal and ethical issues raised and then assess public opinion about its use."
The BMA found it had no "major ethical concerns" over the paying of funeral expenses for a donor although it questioned its effectiveness in increasing donation rates.
"There is also a broader issue about what, if anything, the offer of payment to families in return for donated organs would say about our society's perception of the importance of social solidarity and whether, in reality, that matters," the report adds.
At the end of March 2011, there were 7,800 people on the UK's active waiting list for a transplant, with nearly 3,000 more temporarily suspended from the list because they were currently unfit for a transplant.
© Copyright IBTimes 2025. All rights reserved.





















