Patients who resist malaria infection boost hopes of finding new treatments
Studying sickle cell disease, scientists have come up with a compound to reduce malaria symptoms in mice.
Studying the resistance of sickle cell disease patients to malaria may help scientists come up with new therapeutic alternatives against the disease. A small mice study suggests that it would be possible to target host cells rather than the parasite, as current drugs do.
The 2015 Medicine Nobel Prize rewarded Chinese scientists Youyou Tu for discovery of artemisinin, the substance central to the most effective malaria drugs used today. These medicines have been life-savers, reducing the number of Plasmodiumparasites responsible for the disease in the blood of patients with malaria.
Following this discovery, the number of casualties worldwide has gone down dramatically but in recent years, there has been concern that the parasite is adapting to treatments and that resistance to artemisinin is growing. In coming decades, it might therefore be useful to come up with therapeutic alternatives.
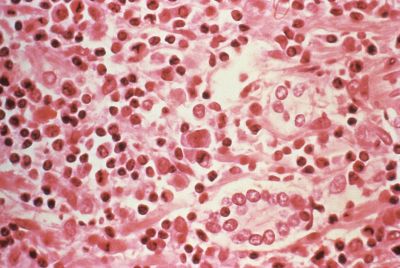
The new study published in Nature Communications began as a research to better understand how sickle cell disease protected people against malaria. "This has been a riddle for 60 years, but in a 2011 study, we began to get clues about this phenomenon. We discovered that when the parasite grows in red blood cells, it establishes its own mode of transporting proteins throughout the host cells", Pr Friedrich Frischknecht, one of the study's author, told IBTimes UK.
"However, in sickle cell disease patients, this mode of transport is altered, leaving them better protected against an infection. This new study was building on this previous one."
Finding the right compound
The scientists, from Heidelberg University Hospital (Germany) have shown that the genetic mutation associated with sickle cell disease lead to an imbalance in agents that chemically combine with oxygen in red blood cells. This alters the interaction between parasites and red blood cells and the transportation of the parasite proteins in the host cells.
The scientists tested a compound in mice to see if they could artificially trigger the same agent imbalance – they used a supplement called menadione. The results were promising as symptoms of cerebral malaria were reduced in rodents. The approach is interesting because it shows malaria symptoms can be reduced by targeting host cells rather than the parasite itself.

This is a small study in mice models however, so it is not clear how far the findings would apply to humans. There is no funding for human clinical trials yet, but the scientists hope to take incremental steps over the next few years to further test this and other compounds – this includes working with parasite strain from the field rather than strains grown in the lab.
"It will likely take some years to test the full potential of these compounds, but we know that the malaria parasite has rapidly acquired resistance to treatment so it is good to stay on top of the game and have therapeutic options ready to investigate", Frischknecht concludes.
What is sickle cell disease?
The term 'sickle cell disease' refers to a group of inherited conditions that affect the red blood cells - the most severe is sickle cell anaemia. Patients have problems because they produce abnormally shaped red blood cells that do not live as long as normal blood cells. Due to their unusual shape, they can also get stuck in their blood vessels.
Sickle cell disease is a recessive condition because the person needs two copies of the mutated beta-hemoglobin gene to have the disorder.
© Copyright IBTimes 2025. All rights reserved.