Suicidal thoughts plague more young people than ever — we must improve child mental health services
One in ten children are affected by a mental health disorder, but many don't have access to professional help.

Britain is facing a child mental health crisis. One in ten children are affected by a mental health disorder. Hospitalisations from self-harm have reached a five-year high. Nearly 80,000 young people and children suffer from severe depression, and 300,000 have an anxiety problem. And without better access to crucial mental health services, the epidemic is reaching a breaking point – more children than ever are ringing the NSPCC's Childline hotline with thoughts of suicide.
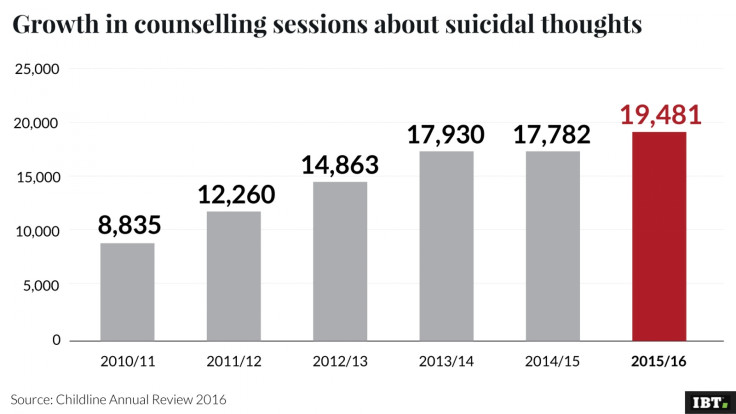
Last year, the charity's service dealt with 19,481 contacts from young people plagued with thoughts of ending their own lives, more than double the number five years ago. School pressures, turbulent home lives and abuse were all cited as triggers for suicidal thoughts – and many of the calls had to be referred to emergency services.
The UK is clearly facing a crisis among its young people. But the failure of services aimed to support the most vulnerable is feeding the crisis. Many of those who called Childline in 2015 were struggling to access professional help, because of long waiting lists, a lack of information or a refusal of help. The NSPCC reported an 87% increase in young people saying they could not access mental health services.
"Not only is it shocking that so many young children are feeling suicidal, but that there is so little help available for them," says Marjorie Wallace, chief executive of the mental health charity SANE. "Currently just one in four children with mental health problems receive any treatment at all, and the Government's new five-year plan for mental health services only aims to increase that to one in three.
"This means children continue to face long waiting times to access often inadequate community or inpatient treatment, or being turned away altogether," Wallace adds. "Even kids in crisis who do find a bed may find it is hundreds of miles away from home and family."
Swingeing cuts to mental health services mean that people in need of professional intervention are being given a watered-down version of support – or no support at all. Research by the charity YoungMinds found that two-third of local authorities in England have reduced their child and adolescent mental health services (CAMHS) since 2010. One council reported a staggering drop of 41% in their budget.
By draining money from children's services, young people are left with no access to early help. As a result, mental health problems can be exacerbated and become more entrenched.
But the blame doesn't lie solely with slashed mental health budgets. Poverty increases the risk of mental health problems. Britain's poorest are suffering the most from austerity policies that have had a detrimental impact on emotional well-being in the UK. Welfare reforms — from the benefits cap to the bedroom tax to the sanctions regime — have led to financial hardship and increased pressure on parents. And this is having a toxic impact on children's mental health.
"I have come across the deleterious effects on children's emotional well-being of parents losing their benefits or being declared 'fit for work' when unwell," one clinical psychologist working in children's mental health services, who did not want to be named, told IBTimes UK.
With services under increasing pressure, it is vital for overstretched mental health services to be fairly funded - or Britain runs the risk of failing a generation of young people.
"If we're serious about improving the mental health of young people, we need a sea change in our approach," says Mark Rowland, director at the Mental Health Foundation. "We need to get away from the 'deficit model' where we wait for mental health problems to develop before taking action to a society that recognises children's mental health as a universal asset to be strengthened and protected."
The Samaritans provides a free support service for those who need to talk to someone in the UK and Republic of Ireland. It can be contacted viaSamaritans.org or by calling 116 123 (UK) or 116 123 (ROI), 24 hours a day, 365 days a year.
More from IBTimes UK
© Copyright IBTimes 2025. All rights reserved.





















