Superbugs will cause 10 million deaths a year by 2050
Antibiotic-resistant superbugs will kill one person every three seconds and cause trillions of dollars of economic damage by 2050 if left unchecked, a review commissioned by the UK government says. Antimicrobial resistance (AMR) – when bacteria change and antibiotics no longer work in people who need them to treat infections – could kill up to 10 million people each year by the mid-point of the 21st century at a cumulative cost to the global economy of $100tn (£69tn, €89tn).
To put this in perspective, cancer kills around 8.2 million people per year at present.
The Review on Antimicrobial Resistance, led by former Goldman Sachs economist Jim O'Neill, recommended a coordinated global effort to cut down on the unnecessary use of antibiotics to tackle dangers posed by superbugs to modern medicine. It also recommended that the pharmaceutical industry be incentivised to promote investment for new drugs and improve existing ones.
The review was commissioned by Prime Minister David Cameron in 2014 to understand and propose solutions to AMR. Currently, around 700,000 people die each year from drug-resistant strains of common bacterial infections, HIV, tuberculosis and malaria.
Big changes
"Fundamental change is required in the way that antibiotics are consumed and prescribed, to preserve the usefulness of existing products for longer and to reduce the urgency of discovering new ones," O'Neill said.
"Governments should be held accountable on this goal to reduce the demand for antimicrobials and in particular antibiotics, as should the main sectors that drive antibiotic consumption: healthcare systems, the pharmaceutical industry and the farming and food production industry."
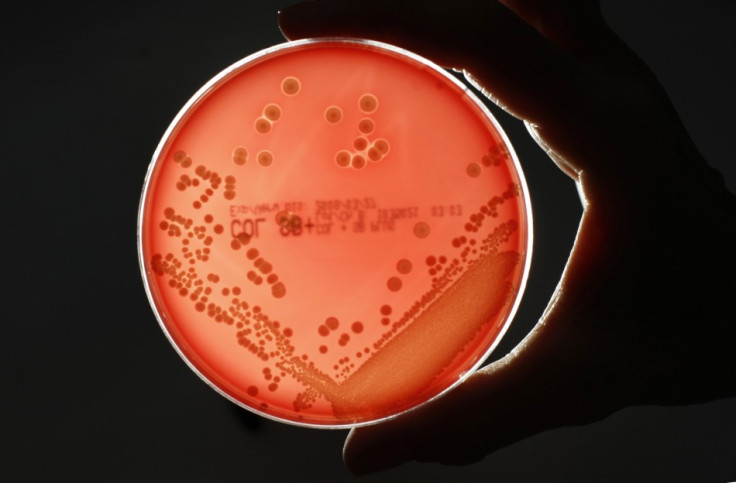
The review estimated that around a third of the 10 million deaths arising from AMR in 2050 will come from drug-resistant E. coli, while a quarter will come from drug-resistant strains of tuberculosis. It added that the 10 million casualty figure is likely to be an underestimate as it does not take into account wider consequences of antibiotics losing their effectiveness on the healthcare industry.
A lack of potent antibiotics could make harmless procedures such as caesarean sections and hip replacements potentially life threatening in the future.
'Massive challenge'
To tackle the problem, O'Neill suggested a "pay or play" system to be applied to the pharmaceutical industry, through which those companies that choose not to invest in research and development towards tackling AMR will pay a small levy to governments. At the same time, companies that invest in R&D and develop new drugs will be rewarded financially to ease their costs.
The review team also estimated that the cost of global action on AMR could run up to $40bn annually over a 10-year period. "This is tiny in comparison to the cost of inaction," they said. "It is also a very small fraction of what the G20 countries spend on healthcare today."
O'Neill added: "Although AMR is a massive challenge, it is one that I believe is well within our ability to tackle effectively. The human and economic costs compel us to act – if we fail to do so, the brunt of these will be borne by our children and grandchildren, and felt most keenly in the poorest parts of the world."
© Copyright IBTimes 2025. All rights reserved.





















