Deadly Australian funnel-web spider venom massively reduces brain damage after stroke in rats
Venom blocks an acid channel in brain responsible for much of the slower-onset damage after a stroke.
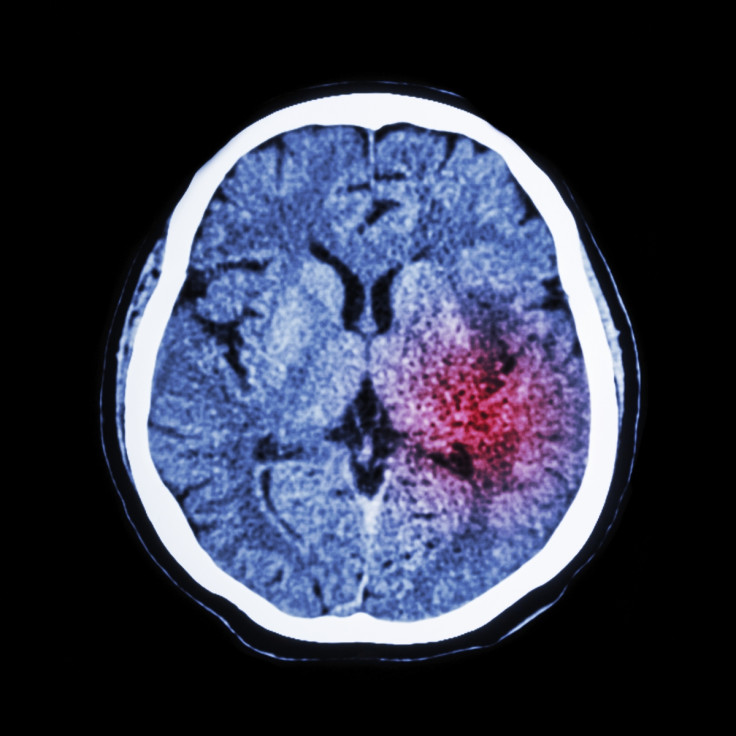
A molecule in the venom of the Australian funnel-web spider could form the basis for the first drug to limit the brain damage that happens in the hours and days after a stroke, finds a study with rats.
Some regions of the brain are killed completely within minutes of a stroke if the blood flow is cut off entirely. But there are often brain regions where blood flow has only been partially blocked. In these areas, cell death is slower, taking a matter of hours to days. This means there is potentially more time for treatment with drugs that could limit the damage.
But at the moment there are no drugs that can help at this stage. Research in rats has now shown that components of the Australian funnel-web spider's venom could be a good candidate for developing the first such drug, according to a paper published in the journal PNAS.
The molecule works by blocking an acid channel in the cell membrane. This channel, called acid-sensing ion channel 1a (ASIC1a), is one of the main components involved in brain damage in the hours after a stroke. Previous studies have shown that knocking out this channel entirely reduces the size of brain damage lesions by about 60% in mice.

ASIC1a is strongly activated during a stroke, when the lack of oxygen to the brain switches the way cells metabolise from a process involving oxygen to one that doesn't involve oxygen. An effect of the oxygen-free process is that it produces acid in the brain, which quickly builds up. The acid activates ASIC1a, which is linked to the brain damage that happens after stroke.
The spider venom molecule – called Hi1a – stops this channel from working if it is given up to eight hours after the start of the stroke.
Deadly or crippling snake venoms are also the target of research for painkillers and even cancer treatments. Tarantula venom has also been investigated as a painkiller, but this is the first time an Australian funnel-web spider's venom has shown promise as a treatment for stroke.
About 6 million people die every year from ischaemic stroke and about 5 million people survive strokes each year, many with a permanent disability, the study authors note. Brain damage after a stroke often leads to a decline in cognitive function and a doubled risk of dementia.

"Despite this massive global disease burden, there are no approved drugs for treating the neuronal injury caused to the brain by the oxygen deprivation occurring during an ischemic stroke," the authors, led by Irène Chassagnon of the University of Queensland, Australia, write in the paper.
"Hi1a is a powerful pharmacological tool for probing the role of ASIC1a in acid-mediated neuronal injury and various neurological disorders, and a promising lead for the development of therapeutics to protect the brain from ischemic injury."
© Copyright IBTimes 2025. All rights reserved.





















