How one woman's quest to cure debilitating chronic pain ended with 'miracle cure' in Brazil

KEY POINTS
- Julia Buckley felt like a carving knife was in her arm and fire ants were crawling on her.
- She travelled to Haiti, Lourdes and Brazil in search of a cure.
- The writer wants to start a #MeToo movement for women's healthcare.
In 2012 travel writer Julia Buckley reached for her coffee to fuel the extra hours she planned to spend at her desk. That simple movement, in a scene familiar to many of us, changed her life forever.
By unwittingly nudging a nerve in her neck, her arm suddenly felt like it was alight and a carving knife had been plunged deep into her armpit, she explained. Months later Buckley, still burdened by these sensations and a debilitating exhaustion, was diagnosed with chronic pain by doctors.
As documented in her new book Heal Me: In Search of a Cure, Buckley spent the next two years lost in the medical system as doctors tried to pin down and treat the cause of her pain. At one stage she took painkillers that made her suicidal. At its worst, the pain prevented her from undertaking simple tasks such as washing her hair.
She was told that there was no cure and that she simply had to learn to cope.
Heavy with the urge to take her own life, she went on a quest for an alternative cure that took her to five continents to test 25 remedies in two years. She took part in voodoo rituals in Haiti, bathed in chicken blood and her own vomit in Soweto in South Africa, visited herbalists in a Chinese mountain village, and was baptised in the grotto in Lourdes.
The pain finally left her body after a ritual by Brazilian spiritual healer João de Deus, or John of God, who was visited by Oprah Winfrey. Buckley managed to escape his eye-scraping technique which he claimed cured sickness but she did undergo "psychic surgery" which involved meditating for hours.
To this day, Buckley does not know what rid her body of the pain - although she suggests it was more likely down to the brain's neuroplasticity rather than any miracle.
What has been made startlingly clear by her story, however, is that chronic pain patients are all too often left to deal with never-ending pain and there is an unconscious bias among some clinicians that means that women and people of colour do not receive adequate healthcare because they are not believed.
She spoke to IBTimes UK about starting a #MeToo movement for healthcare, why she does not encourage anyone to seek a miracle cure, and the touching messages she has received from fellow chronic pain sufferers.
IBT: What was it like living in constant pain for four years?
JB: It was soul-destroying and life-destroying. It felt like being in a limbo. It's not your life as you know it and you're told there's no chance of getting it back. You're in this weird netherworld between the sick world and the normal one. No one can see your illness so you look totally normal and so people don't understand. It's like being a ghost.
IBT: How would you describe the pain that you felt?
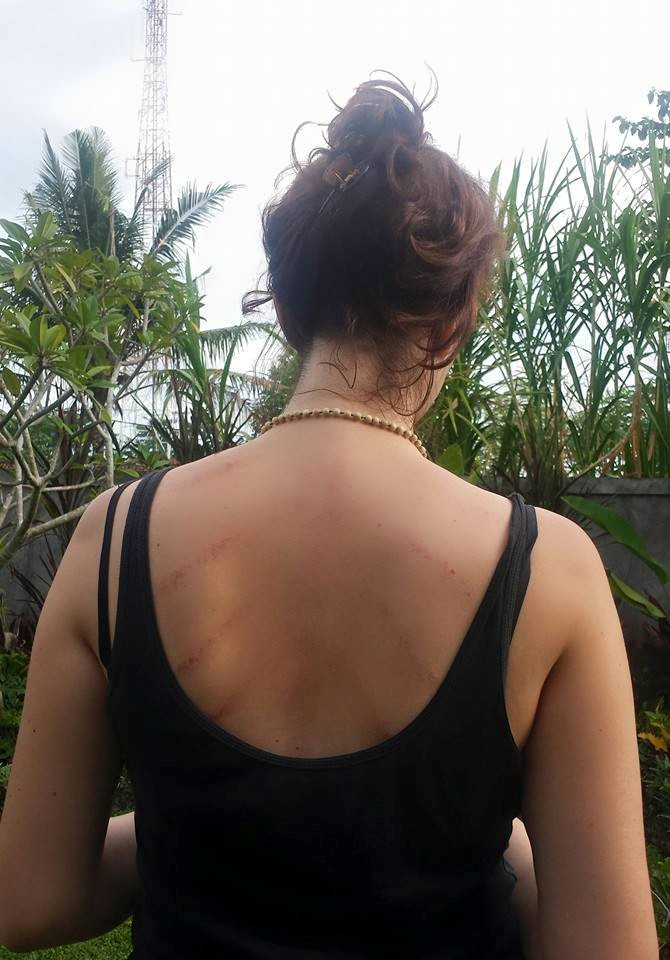
JB: There was an all-over aching muscle pain and then it felt a carving knife in my armpit. It felt like my arm was on fire and fire ants were crawling up my arm. There was a bonfire burning inside my right shoulder blade. I had a terrible neck pain and general arthritic aching all over. It was coupled with absolute exhaustion. It meant when you do get energy to do something like go to shops or watch TV you are exhausted by it.
Everyone has had pain so everyone thinks they know what chronic pain is. When someone looks "normal" and says they are in pain permanently you can't help but think they are exaggerating it. I lost a lot of friends because they didn't believe me or I didn't like how they were responding. Only my mum really believed me. It was really isolating, and you have to be aware of presenting yourself to people the whole time. You think 'do I look sick enough and what will people think if I enjoy this glass of wine?'

IBT: How did it feel being told there was no cure?
JB: Devastating. I was told I was going on a pain management course for three weeks, expecting to be cured and working out solutions. On the first day they sat us all down and said there is no cure and you won't get better. This is about managing despite the pain. I was told I was too angry and I was told I'd come on the course too early because I hadn't accepted my diagnosis. It was like having my life taken away. I had been condemned to living death the rest of my life. The fact that people with chronic pain are 14 times more likely to commit suicide speaks for itself.

IBT: What do you want people to take from the book?
JB: I'd like to start a dialogue. If one third of people have chronic pain we all know someone who has it. I want to start a conversation about how women are treated by the healthcare system. I don't know if it was John of God or some switch that was flipped in my brain or if it was a placebo or some domino effect that kept rolling, but I did get better and that's the important thing. There is hope. People with pain are told there is literally no hope. You life is over. And I don't think that's true. If it could help one person to make them feel better whether mentally or physically it would all be worth it and if one person could be cured completely I would do it all again.
This is now an extension of #MeToo and Times Up, and an examination of women's place in society. I would like to talk about women's health like we talk about sexual assault.
IBT: What was it like writing the book? Have you been contacted by anyone with chronic pain?
JB: It has been really overwhelming. The only reason I wanted to do it in was I had a chance to give a voice to the 28 million people who have chronic pain.
I woke up today to one woman tweeting me to say it had put things on a page that she had not wanted to confront before, and that she felt she had a new way forwards. And that is overwhelming. A guy tweeted me to say he was reading it and it felt like it had been written to him and he felt he wasn't alone.
That is so important with an invisible illness. If someone has a terrible diagnosis or a heart attack it's easier to ask how are you doing. A lot of people feel as low as I was feeling. The suicide rates show that. These stories aren't normally told. It's not sexy or glamorous. There are no coffee mornings in aid of us.





IBT: At a time when there is a lot of anti-science and anti-expert sentiment and people dismissing conventional medicine for healing, were you wary of balancing this in the book?
JB: I felt a huge responsibility and had so much stress exactly because of that. I didn't want to go too far either way. At the moment in the UK we are so polarised with the NHS. It's as if medicine and science is the NHS, and either you love it or want to dismantle it. There's no room in between.
I think the NHS is extraordinary and doctors save lives every day. But people are being failed and the methods for treating chronic pain are shown to be outdated. In the '90s you would hand out opioids and then we realised that didn't work - but now we've gone too far the other way.
Evidence is coming out at the cutting edge that is showing you can retrain your brain, and obviously it takes years to filter down to a GP level - and it's killing people in the meantime. We need to talk about bedside manner: studies show that can affect the outcome of the treatment or operation, and pain levels or blood pressure can be affected by just how you get on with your doctor.
Equally I don't want people to read it and think they should go to Brazil for a miracle cure. Someone heard me on the radio and said they wanted to go to Brazil to see John of God. But it's not about John of God. I still don't know what happened and you have to really do some work on yourself. And you should always stay in touch with your doctor and find a doctor who understands you.
IBT: You book speaks a lot about Yentl syndrome and how women and people of colour are treated differently by clinicians. How can we change this?
JB: A lot of it comes down to training. Any kind of company has an unconscious bias. It doesn't help that most doctors are middle-aged men who have a certain view of women. It's really hard because a part of what doctors do is they need to be emotionally disconnected. But I think they need to remember that what for them is an eight-minute appointment is an important part of someone's life.
They need to see women as individuals and not "the woman with bad arm in cubicle two". Women die from heart attacks because the symptoms present different to men's. And I think it's a systemic thing that needs to be hammered in at training. They need to be more aware.





















