Priority pathogens: The antibiotic-resistant bacteria WHO says pose the biggest threat to humans
Academics and drug companies have been urged to focus on finding new antibiotics for 12 families of resistant bacteria.

The World Health Organization has released a list of 12 families of antibiotic-resistant bacteria that are the biggest threat to human health.
The bacteria are grouped into three categories according to the threat they pose, from medium to critical. The list includes multiple-resistant Staphylococcus aureus (MRSA), multiple-resistant bacteria that cause gonorrhoea and "nightmare" multiple-resistant Enterobacteriaceae.
The list is intended to focus medical research efforts on new antibiotics for these bacteria, said Marie-Paule Kieny, WHO assistant director-general for health systems and innovation. Pharmaceutical companies directed by market interests alone will not be enough to tackle the problem of antibiotic resistance, she said at a press conference.
"There is somewhere a market failure," Kieny said. "If we want to develop new antibiotics it [should not be] to use them like the previous ones so that resistance grows so quickly that in a number of years they have no use any more."
Directing scientific and pharmaceutical research towards the most urgently needed antibiotics was one part of the strategy required to tackle antibiotic resistance, with other aspects including financial incentives for drug companies for developing new antibiotics.
How were they ranked?
The WHO ranked the bacteria according to threat by how deadly they were, the length of hospital stay required during an infection, how often they are resistant to antibiotics, how easily they spread between animals, from animals to humans and between humans, and how preventable they are, how many alternatives to antibiotics there were, and whether there are new antibiotics targeted at them in the pipeline.
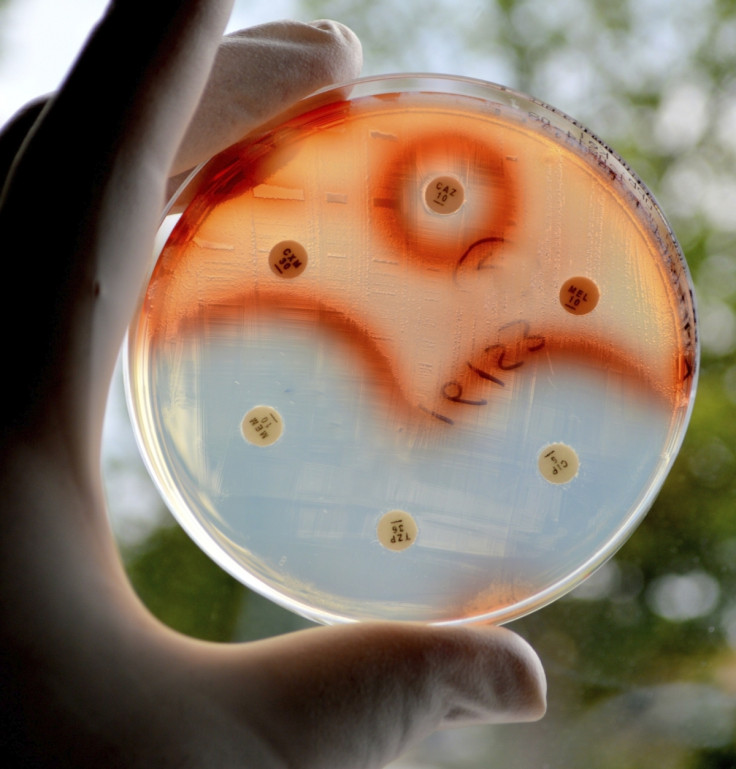
The bacteria that pose the biggest threat
Priority 1: Critical
- Acinetobacter baumannii, carbapenem-resistant
- Pseudomonas aeruginosa, carbapenem-resistant
- Enterobacteriaceae, carbapenem-resistant, ESBL-producing
Priority 2: High
- Enterococcus faecium, vancomycin-resistant
- Staphylococcus aureus, methicillin-resistant, vancomycin-intermediate and resistant
- Helicobacter pylori, clarithromycin-resistant
- Campylobacter spp., fluoroquinolone-resistant
- Salmonellae, fluoroquinolone-resistant
- Neisseria gonorrhoeae, cephalosporin-resistant, fluoroquinolone-resistant
Priority 3: Medium
- Streptococcus pneumoniae, penicillin-non-susceptible
- Haemophilus influenzae, ampicillin-resistant
- Shigella spp., fluoroquinolone-resistant
What is antibiotic resistance?
Some bacteria are not killed by the antibiotic treatments that have been designed to kill them. These bacteria are said to be antibiotic resistant. Bacteria can be resistant to one antibiotic or to several. Some lethal bacteria are resistant to all medically approved antibiotics.
Antibiotic resistance is a trait that bacteria develop by evolution. When bacteria are exposed to an antibiotic, the ones that the drug can successfully kill all die off. But in a population of bacteria – which could be as large as trillions of individual bacterial cells – there could be just one or two that have a genetic mutation that gives them resistance.
When all the susceptible bacteria die off, the ones that have resistance will be able to thrive. These can be spread between humans or the animals that they infect, and previous antibiotic treatments will no longer be effective.
The next step is to use another antibiotic that works in a different way. However, when exposed to a new antibiotic, the bacteria can go through exactly the same process again. This can result in multiple-resistant bacteria such as MRSA.
© Copyright IBTimes 2025. All rights reserved.





















