UK underperforming on treatable health conditions, new report shows
The King's Fund, an independent think tank involved with work relating to the health system, said the UK health system's poor performance on avoidable deaths should be a serious concern for political leaders and policy-makers.
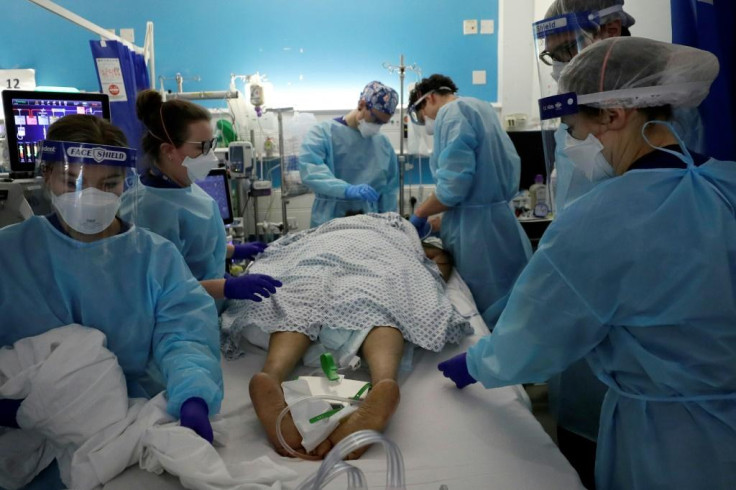
The UK is underperforming on treatable health conditions, a new report has shown.
The King's Fund, an independent think tank involved with work relating to the health system, said the NHS' poor performance on avoidable deaths should be a serious concern for political leaders and policy-makers.
According to their research, the NHS' below-par provisions were a result of "strikingly low levels" of clinical staff and equipment.
It found that the UK has fewer doctors and nurses per head than most comparable countries, and is more heavily reliant on internationally trained staff.
Britain has just three doctors per 1,000 people, for example, while Greece has 6.3 doctors per 1,000 people.
As a result, the UK has among the lowest levels of life expectancy for men and women, with falls having been particularly striking since the pandemic.
The research showed that the UK suffered from higher levels of deaths from treatable diseases such as heart attack and stroke than the majority of similar countries, and below-average survival rates for many common cancers.
However, the report did stress that life expectancy is determined by other factors as well as healthcare.
An understaffed NHS is a problem exacerbated by a sharp rise in striking workers over the past year – just last week hospital doctors staged a 72-hour walkout over what they describe as a "26 per cent pay cut over the previous 15 years".
The British Medical Association, who organised the strike, said they would stage further protests in the coming months if the government sticks to its five per cent offer.
It appears unlikely that a solution will be found over pay in the short-term, after the Bank of England raised interest rates for the 13th time in a row last week, in response to elevated inflation levels across the country.
The performance of Britain's taxpayer-funded health system has been under particular scrutiny as waiting lists for treatment reach record levels ahead of a general election in which it is likely to be a pivotal issue for voters.
The service has been increasingly stretched for funding, resources and staff in recent years, a situation exacerbated by the impact of the COVID-19 global health crisis.
Prior to the pandemic in February 2020, there were already 4.43 million people on a waiting list for care.
At the beginning of the pandemic, the combination of suspension of non-urgent services and changes to individuals' behaviour meant that the number of people joining the waiting list initially dropped.
However, this has since been rising - and despite some improvements earlier in the year, waiting times remain far higher than pre-COVID.
The latest figures for April 2023 show that around 7.42 million people waiting for treatment, a slight increase on the previous month; nearly 3.09 million of these patients waiting over 18 weeks, and around 371,000 of these patients waiting over a year for treatment – which is around 292 times as many as in March 2019, before the pandemic began.
The King's Fund report supports the view that the Pandemic hit treatment waiting times far harder in the UK than in other countries.
It suggests that the pressures of the pandemic compounded the consequences of more than a decade of squeezed investment in staff, equipment and wider services.
This has led to a worrying backlog, at a time when the nation already faces a cost-of-living crisis, putting further strain on the health service.

And a recent poll revealed that Britons believe Prime Minister Rishi Sunak is failing to deliver on his promise to "cut waiting lists" across the NHS.
It also found that the nation's top priority was easing the cost of living – 59 per cent listing it as important – followed by ensuring people can get NHS treatment more quickly (54%) and reducing NHS waiting lists (51%).
So what is the solution?
Working to improve the existing health system while providing it with the "adequate resources, political support, and long-term planning" it desperately needed would give the NHS the best chance of delivering "the timely, high-quality care and outcomes it is capable of", the report concluded.
On Sunday, Sunak declared that the NHS is poised to undergo the "largest expansion in training and workforce" in its history.
He is referring to the long-delayed "NHS Workforce Plan", set to be published later this week. The document will detail an increase in "doctors, nurses and GPs," Sunak said.
It follows last week's announcement that £21 million would be invested in AI developments across the health service, allowing NHS Trusts to accelerate the deployment of the most promising AI tools across hospitals, to help treat patients this coming winter.
The Health and Social Care Secretary, Steve Barclay, has also committed to rolling out AI stroke-diagnosis technology to 100 per cent of stroke networks by the end of 2023 – up from 86 per cent today – helping thousands of patients suffering from a stroke get treated faster.
According to Barclay, AI tools are "already making a significant impact" across the NHS, through diagnosing conditions earlier.
He says he is now focused on "adopting" the latest cutting-edge technology across the health and care system to "ensure we can continue to deliver the best care for our patients and cut waiting times" – one of the government's five priorities.
© Copyright IBTimes 2025. All rights reserved.





















