Ebola rapid test kit finds no takers despite approvals
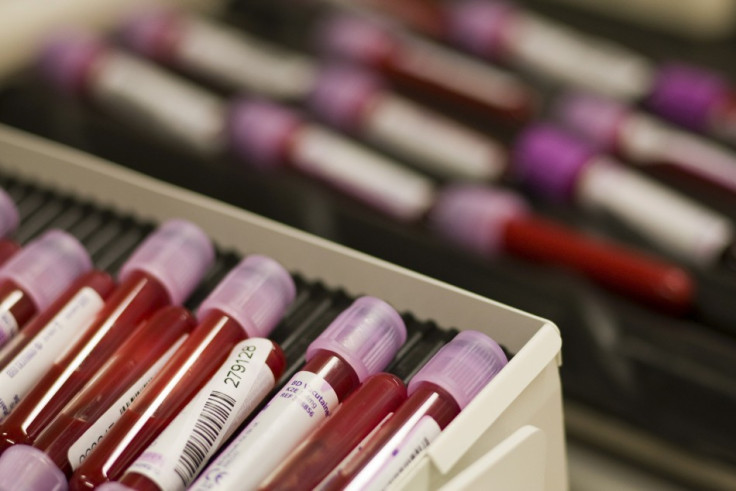
A rapid test that diagnoses Ebola rapidly at the bedside, and is as sensitive as the conventional laboratory-based method, has found no takers despite approval by the World Health Organization and the US Food and Drug Administration.
With Ebola refusing to die down and 24 confirmed cases reported in Guinea and Sierra Leone in the week ending 14 June, the kit would allow workers to identify infected people and isolate them faster, before lab-based tests can be done, says Nahid Bhadelia, an infectious-diseases physician at the Boston University School of Medicine and the Boston Medical Center in Massachusetts.
People who were infectious were going undetected for five or six days before being diagnosed by lab diagnostics which takes time.
The kit detects Ebola-specific proteins (antigens) in the blood and is as sensitive as the standard polymerase chain reaction (RT-PCR) test that amplifies and detects Ebola-specific genetic sequences in blood and other bodily fluids.
Regulatory delays
But four months after approval, the kit has not yet been deployed due to delay by national regulators.
"A lot of people are frustrated," says Nira Pollock, an infectious-diseases researcher at the Boston Children's Hospital in Massachusetts, and senior author of an independent field-validation study of the test kit, published on 26 June in The Lancet.
Researchers from Harvard Medical School, Partners In Health and Boston Children's Hospital were involved in the study.
Both rapid diagnostic tests, on whole blood, and RT-PCR, on plasma, were also performed on 284 samples in the laboratory. The rapid diagnostic test detected all confirmed cases of Ebola that were positive by the benchmark test with a sensitivity of 100%.
The test, developed by Colorado-based medical-diagnostics company Corgenix, is simple enough to be used by healthcare workers with minimal training in remote villages.
Robert Garry, a virologist at Tulane University in New Orleans, Louisiana, blames the delays on what he says are overly restrictive and ambiguous sets of guidelines released by WHO in March and June.
They state, for example, that the rapid "antigen-detection" tests "have no role in the routine management of Ebola in settings where PCR (molecular) testing is available; however, they may have utility in settings without laboratory infrastructure if their benefits and limitations are understood".
Additional decentralised testing is needed in places where outbreaks occur to slash delays in identifying those infected, he says.
"We need to rethink the conventional wisdom about PCR being the only answer," he adds.
Mark Perkins, chief scientific officer of the non-profit organization Foundation for Innovative New Diagnostics (FIND) in Geneva, Switzerland, defends the WHO guidelines noting that rapid tests for antigens report too many false positives.
In the independent validation, six out of 77 people who tested negative for Ebola using PCR were declared positive by the Corgenix kit. "To roll out an assay with so many false positives is unthinkable," Perkins says. Rapid tests are now of "reduced relevance", he adds.
But Bhadelia and others would like to use the test to speed up early identification and do not discount the role of lab tests.
They in turn point to the study which showed some of the results from PCR tests identified as negative were later confirmed positive as shown by the Corgenix kit.
© Copyright IBTimes 2025. All rights reserved.




















