Threat to global health feared over drug-resistant malaria seen at Myanmar-India border
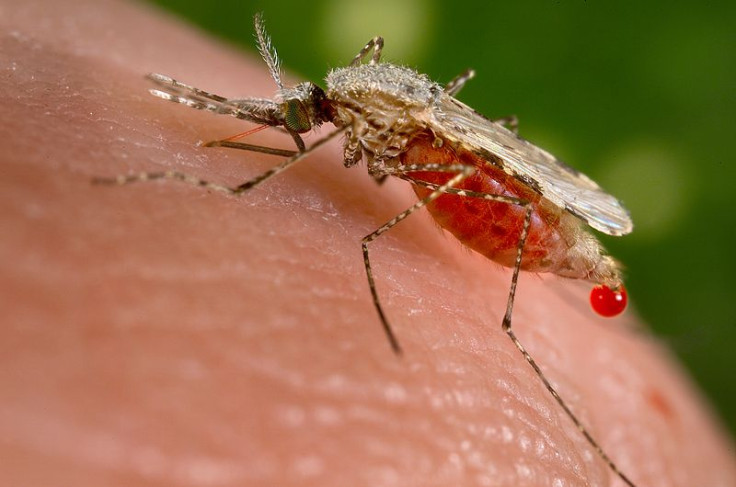
Drug-resistant malaria detected at the Myanmar-India border could pose a threat to millions across the globe if the resistance spreads beyond, scientists say.
"Myanmar is considered the front line in the battle against artemisinin resistance as it forms a gateway for resistance to spread to the rest of the world," said Charles Woodrow of the Mahidol-Oxford tropical medicine research unit, who led the study at Oxford University.
In the study, published in The Lancet Infectious Diseases journal, Woodrow's team collected 940 parasite samples from 55 malaria treatment centres across Myanmar and its border regions.
Almost 40% of the samples showed mutations in the bacteria's kelch gene, K13, showing clear signs of artemisinin drug resistance.
They also confirmed resistant parasites in Homalin, in the Sagaing Region, only 25km from the Indian border.
Deaths from mosquito-borne malaria have nearly halved since 2000, but the infection still killed about 584,000 people in 2013, mostly in Africa, according to the World Health Organization (WHO).
Much of the success in fighting the disease was due to the use of combination therapies (ACTs) based on artemisinin, a Chinese herb derivative.
But now with the malaria parasite building up resistance to the drugs, prospects of a global resurgence of the bacteria and threat to health are high.
Cambodia, Thailand, Laos and Vietnam
Before being identified in Myanmar in 2008, signs of resistance were found in Cambodia and since have also been confirmed in Thailand, Laos and Vietnam, according to the WHO.
Myanmar, which has the largest malaria burden in the South East Asia region, is the latest frontier in the spread of resistance to artemisinin, with experts warning of huge economic and human costs if allowed to spread.
A study published in the Malaria Journal last year had estimated an extra 116,000 deaths per year if artemisinin resistance is not stopped. Medical costs could exceed £21m ($32m) per year, while productivity losses from a rise in cases and deaths are estimated at £250m ($385m).
Back in the last century, chloroquine saved hundreds of millions of lives, but resistance was discovered in 1957 around the border between Cambodia and Thailand.
Resistance spread around the world and reached Africa 17 years later.
Chloroquine was then replaced by sulphadoxine-pyrimethamine (SP), but resistance to SP subsequently emerged in western Cambodia and again spread to Africa.
SP was replaced by artemisinin combination treatment, or ACT.
The rise of resistance to both chloroquine and artemisinin in South East Asia is being ascribed to lower levels of natural malaria immunity in the region than in Africa.
Mike Turner, the head of infection and immunobiology at the Wellcome Trust medical charity, told BBC: "The new research shows that history is repeating itself, with parasites resistant to artemisinin drugs, the mainstay of modern malaria treatment, now widespread in Myanmar.
"We are facing the imminent threat of resistance spreading into India, with thousands of lives at risk."
© Copyright IBTimes 2025. All rights reserved.



















