World Malaria Day 2017: The long path to find a vaccine against one of world's greatest killers
Finding a vaccine would help eradicate malaria once and for all.
Often referred to as one of the world's biggest killers, malaria remains endemic in 91 countries around the world. But in the last two decades, the fight against the disease has started to pay off, leaving the global health community cautiously optimistic that the disease may one day be eradicated.
Since the turn of the century, the number of people dying from malaria has been greatly reduced, with the mortality rate being cut down by 62% between 2000 and 2015.
The development of effective antimalarial drugs, combined with the roll-out of robust preventive actions, including the use insecticides and mosquito nets have helped save millions of lives. But one crucial tool is missing in the fight against the disease – a vaccine.
Scientists have been working on this for decades, but this work has proven more challenging than expected.
In late 2016, the World Health Organisation announced that the world's first malaria vaccine – known as RTS,S – would be rolled out in pilot projects in three countries of sub-Saharan Africa, after recent advanced clinical trials showed that it could provide infants with partial protection against the disease.
However few experts believe that this vaccine will be the answer that the world needs to eradicate malaria once and for all.
The need for a vaccine
In 2015, Chinese scientist Youyou Tu received the Nobel Prize in Medicine for her discovery of artemisinin nearly fifty years before. Artemisinin combination therapy is today the world's first-line treatment against malaria and it has been instrumental in reducing the malaria death toll.
However, resistance to these antimalarial drugs is now growing, while prevention strategies are not 100% effective. Mosquito bed nets for instance can only protect people at night, but the most common species of mosquitoes tend to feed at dawn or at dusk.
"In some areas where the level of malaria transmission is not too high, we can probably get rid of malaria without using a vaccine. There are success stories, for example Sri Lanka, which became the last country to eradicate malaria with drugs, insecticides and nets. But in some areas, in particular in Africa and in the Sahel, this may not be enough. We are going to need new tools, one of which will have to be a vaccine", Brian Greenwood, professor of Clinical Tropical Medicine at the London School of Hygiene and Tropical medicine told IBTimes UK.
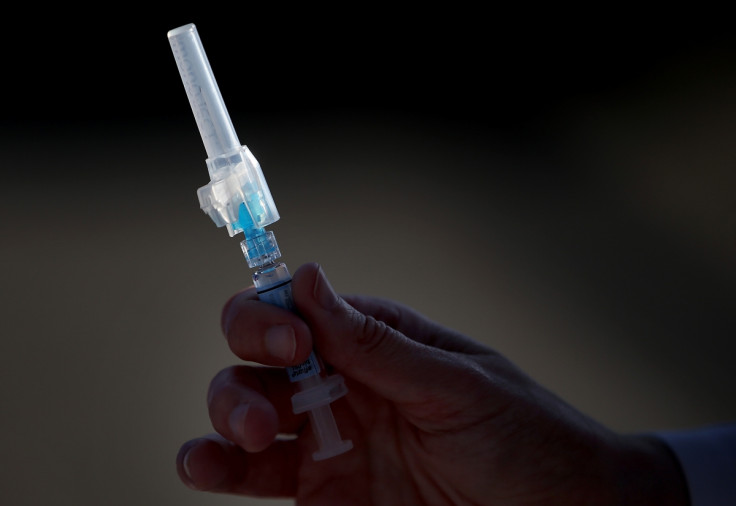
Historically, many infectious disease – like polio or smallpox – have been eradicated with immunisation. But finding a vaccine for malaria is a different story.
The complex biology of the malaria parasite and its great genetic diversity are impediments to malaria vaccine efficacy. Furthermore, the parasite's life cycle comprises different stages of infection. When the parasite is transmitted to humans by an infected mosquito, it first establishes an asymptomatic liver stage infection that is followed by a symptomatic blood stage infection. Questions remain about which stage of the parasite's life cycle a vaccine should target.
Greenwood adds: "A simple virus will have only one way it get into a red blood cell and if you can stop it, then that's the end of it. But the malaria parasite may have several ways to infect your cells, so even you block one, it may use another. This is an clever, adaptable parasite".
Funding limitations and lack of consensus within the field of malaria research have also at times been problematic.
"Efforts to find a vaccine for malaria have been slow. Over the years, some vaccines candidates have gone forward to trials, even though there was not enough evidence that they worked. " Stefan Kappe, from the Center for Infectious Disease Research and University of Wahington, tells IBTimes UK.
The promise of RTS,S
RTS,S is the world's most advanced vaccine candidate against the most deadly form of human malaria, P. falciparum. It works by preventing the parasite from infecting and multiplying in the liver, after which it would normally re-enter the bloodstream – leading to the emergence of malaria symptoms.
The final results of clinical trials, published in 2015, suggest it provides partial protection against malaria. Vaccine efficacy against clinical malaria for babies aged aged 6-12 weeks was 36% for those who received a booster dose. In infants aged between 5 and 17 months old, efficacy was about 26%. However, the protection conferred by the vaccine was found to rapidly decline.
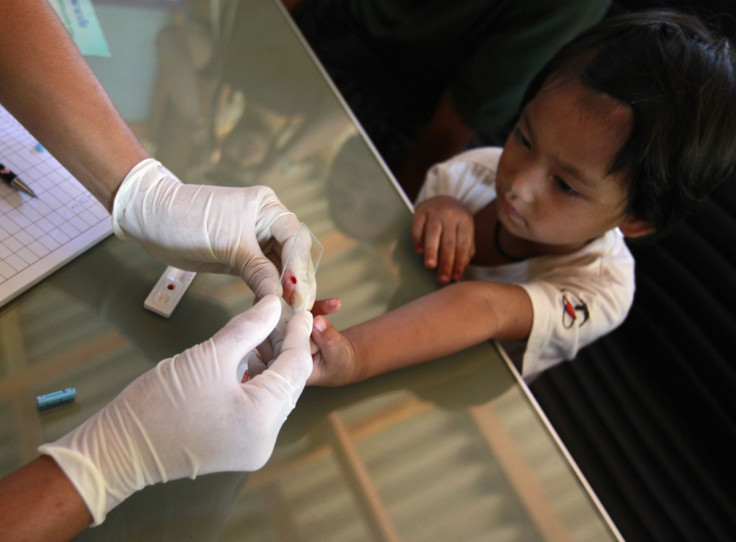
Given those findings, most scientists agree that malaria won't be eradicated with RTS,S alone. However, the vaccine may still save some lives in the worst affected regions and could be a useful complement to existing tools.
"RTS,S is not a miracle solution. It's not good enough to justify giving it to everybody, as part of a routine vaccination program. In some countries that are already doing quite well with current tools, using it may not be a cost-effective approach", Greenwood says. "But there are some areas in Africa and Sahel where malaria is not controlled and where it could save some lives".
The whole parasite
Other vaccines currently being investigated may hold more promise. In the early days of malaria vaccine research, scientists had shown that immunisation with irradiated-attenuated sporozoites (the form of the parasite the mosquito injects when it bites) could protect against infectious sporozoites. This result was subsequently confirmed in humans.
Vaccines containing live parasites – weakened so that they cannot harm people and targeting the parasite when it's in the liver – seem to be one of the best approaches, but it's only recently that scientists have began to test it seriously again.
In his lab, Kappe and his team have gone down this route, but instead of weakening the parasites with irradiation, they have resorted to genetic engineering. They showed that deleting 3 genes from the parasite arrests it in the liver and creates a strain that is safe for use in vaccination. The results were recently published in the journal Science Translational Medicine.
Another study recently published in the journal Nature also tested a vaccine containing live sporozoites. Instead of weakening the parasites, scientists provided patients with antimalarial drugs to protect them during vaccination. During this trial, all of them were protected against a subsequent malaria infection.

There is hope that all these innovative initiatives will lead to a more effective vaccine than RTS,S, but it is certain that this will take time.
"On one hand, having RTS,S is great because it shows us that it can be done, it is possible to develop a vaccine for malaria. But it's important to make sure that it does not overshadow all the other initiatives taking place, as some of them could lead to the development of next generation, more effective malaria vaccines - and to the eradication of malaria" Kappe says.
© Copyright IBTimes 2025. All rights reserved.





















