3D Printer Builds Living Tissue - Without Problems of Stem Cells
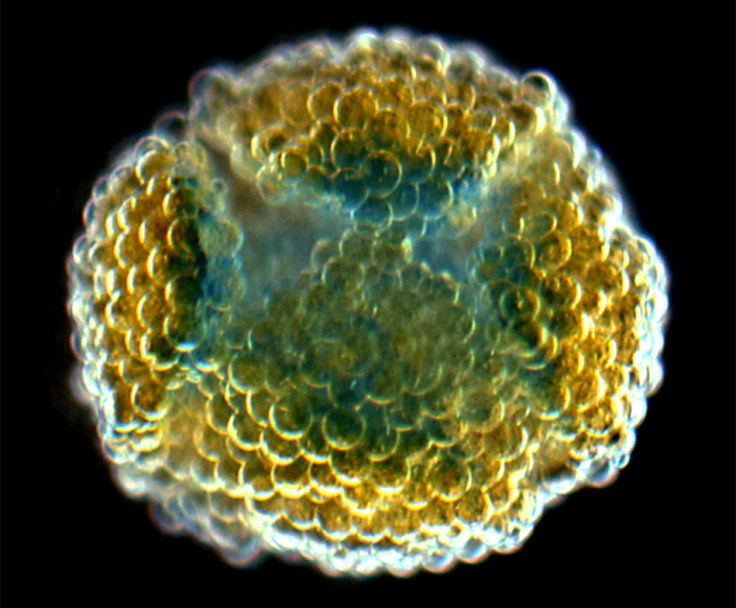
Scientists at Oxford University have developed a 3D printer that can create living tissue without the problems associated with stem cells.
The custom-built machine is able to print materials that share several of the properties of living tissues and can perform some cellular functions.
The material consists of thousands of connected water droplets that are encapsulated in lipid films - a membrane that forms a barrier around cells.
Researchers say these printed "droplet networks" could be used as the building blocks for delivering drugs to places they are needed, or to replace or repair damaged human tissue.
Research leader Professor Hagan Bayley said: "We aren't trying to make materials that faithfully resemble tissues but rather structures that can carry out the functions of tissues
"We've shown that it is possible to create networks of tens of thousands of connected droplets. The droplets can be printed with protein pores to form pathways through the network that mimic nerves and are able to transmit electrical signals from one side of a network to the other."
Previously, scientists have been able to print clusters of the embryonic stem cells through 3D printers. Researchers at Heriot-Watt University in Scotland said the technology has the potential to revolutionise organ replacements.
However, with cells that contain genetic material, there is always the possibility of it malfunctioning - it can replicate or be rejected by the body.

The Oxford University researchers say the tissues from their 3D printer are entirely synthetic, have no genome and do not replicate.
Because they have no genetic material, they are able to avoid problems with other artificial tissues, such as stem cells.
Each droplet is about five times larger than living cells, but the researchers say there is no reason why they could not be made smaller.
The 3D printer was built by Gabriel Villar, a student in Bayley's group and lead author of the study.
"We have created a scalable way of producing a new type of soft material. The printed structures could in principle employ much of the biological machinery that enables the sophisticated behaviour of living cells and tissues," he said.
The droplet networks remain stable for weeks and can be designed to fold themselves into different shapes after printing.
This means a flat shape that looks like the petals of a flower can be programmed to fold in on itself to create a hollow ball.
Similar to muscle movement, the folding is powered by osmolarity differences that cause water transfer between individual droplets. Osmolarity is the measure of solute concentration.
Bayley said: "Conventional 3D printers aren't up to the job of creating these droplet networks, so we custom built one in our Oxford lab to do it.
"At the moment we've created networks of up to 35,000 droplets but the size of network we can make is really only limited by time and money. For our experiments we used two different types of droplet, but there's no reason why you couldn't use 50 or more different kinds."
© Copyright IBTimes 2025. All rights reserved.