Anorexic teenage student starved to death after catalogue of NHS failures
Averil Hart was failed by numerous NHS bodies responsible for her care, report finds.

A 19-year-old student with anorexia starved to death in a matter of weeks after a series of NHS failures, a scathing report has found.
Averil Hart's death in December 2012 was an "avoidable tragedy" that could have been prevented had the appropriate care been provided, the Parliamentary and Health Service Ombudsman found.
"Several NHS organisations missed opportunities to prevent the deterioration which led to her final admission to the hospital where she died," its report on Friday (8 December) said.
It found the four NHS bodies responsible for her care were also "defensive or protective" of themselves when family members tried to get answers following Hart's death.
It warned the case highlighted the widespread problems with adult eating disorder services in the NHS.
The scathing criticism saw Hart's family, from Sudbury in Suffolk, condemn the treatment she suffered.
Father Nic Hart, managing director of a weather experiment firm in Essex, who spent £200,000 investigating his daughter's death, told the Daily Mail: "The care that Averil received was Third World – they left a high-risk patient to fend for herself.
"Not only was the care that Averil received negligent, but the investigation of her death took far too long and this has resulted in further unnecessary deaths."
Hart, the youngest of three sisters, had a three-year history of anorexia nervosa when she became unwell after her A-levels.
Severely underweight, she was admitted to the Eating Disorders Unit in Cambridge aged 18 in September 2011.
The following 11 months saw her gain weight and she was discharged in August 2012 so she could study English and creative writing at the University of East Anglia.
Her care was taken on by the university GP service and outpatient eating disorder services in Norwich, with discharge notes warning she needed ongoing monitoring and was "vulnerable to subsequent relapse".
But Hart was badly failed by NHS services, the ombudsman report found.
The mistakes higlighted included:
- Discharge notes failing to highlight the urgency of invoking a contingency plan if she deteriorated;
- Not being appointed a care coordinator by Norwich eating disorders service for a month;
- Not being seen weekly by the university GP service, with one locum GP telling her at her last appointment on 8 November "she did not need to come back for a month".
When her father and older sister, Imogen, visited her on 28 November "they were shocked by how much weight she appeared to have lost".
By December, Hart weighed just 4st 10lb having lost nearly a third of her body weight since September.
Despite her family members seeking emergency help, she was found collapsed in her university accommodation on 7 December.
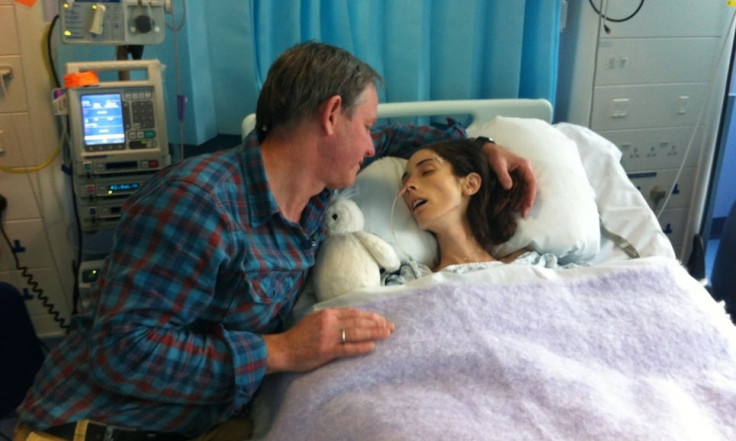
Failures persisted when she was taken to Norfolk and Norwich University Hospital and later transferred to Addenbrooke's Hospital in Cambridge.
She died on 15 December having suffered severe brain damage due to dangerously low blood glucose levels.
The report into her death said: "There were multiple opportunities between August and December 2012 to identify what was happening to Averil, to intervene to remedy the situation at that time, and therefore to prevent the subsequent course of events that led to the final emergency admission to hospital which culminated in her death."
It called for junior doctors to be trained about eating disorders as well as greater provision of eating disorder specialists.
Better coordination of care between NHS organisations treating people with eating disorders was also needed, it added.
A Department of Health spokeswoman said: "We are introducing the first ever eating disorder waiting time standards and investing £150m creating 70 new community eating disorder services across the country, so that no-one will have to go through the same ordeal as Averil."





















