Is HIV hiding in your brain? MRI scans can identify virus from changes to white matter
People with HIV may suffer from cognitive problems directly tied to presence of virus in the brain.
HIV can persist in the brain of patients, even when the disease is kept under control by effective treatments. Doctors can spot the presence of the virus in the brain on MRI scans, identifying changes to people's white matter, a new study has shown.
There is growing evidence that HIV can continue to replicate in different parts of the body even when people are taking suppressive antiretroviral therapy (ART) – including in the cerebrospinal fluid, the clear fluid found in the brain and the spine.
Detectable HIV in the cerebrospinal fluid is hypothesised to increase the risk of neurological problems.
Before effective treatments were designed against HIV, a significant proportion of patients went on to develop dementia. The situation has greatly improved since then, but a number of patients still report problems.
"Today, up to 50% of patients present some kind of neurological symptoms despite taking ART – ranging from memory impairment and issues with concentration to weakness in their arms and legs. These problems are directly linked to the presence of HIV in the cerebrospinal fluid in 10 to 15% of cases. The issue is that we only have invasive methods to test whether HIV is present and the cause of the cognitive problems observed", senior author Professor Ravi Gupta (UCL Infection & Immunity) told IBTimes UK.
At present, doctors have to perform a lumbar puncture to confirm whether HIV is in the cerebrospinal fluid of people who experience cognitive problems – inserting a needle into the back to draw out the spinal fluid and putting them in hospital for several hours.
Using MRI scans
In the study, now published in the journal of Clinical Infectious Diseases, the scientists have shown that traces of the virus in the brain could also be identified with MRI scans, potentially changing the way patients with cognitive problems due to HIV are taken care of.
The team looked at data from 146 HIV patients who had been investigated for cognitive problems between 2011 and 2015. The scientists found that HIV was active in the brain of 15% of these patients.
Using MRI scans, they honed in on signs of white matter changes in the brain, showing that such changes could make it ten times more likely for the virus to be present in cerebrospinal fluid.
These white matter alterations are known as diffuse white matter signal abnormalities. They are linked to cognitive problems and can be triggered by inflammation in the brain caused by HIV infection.
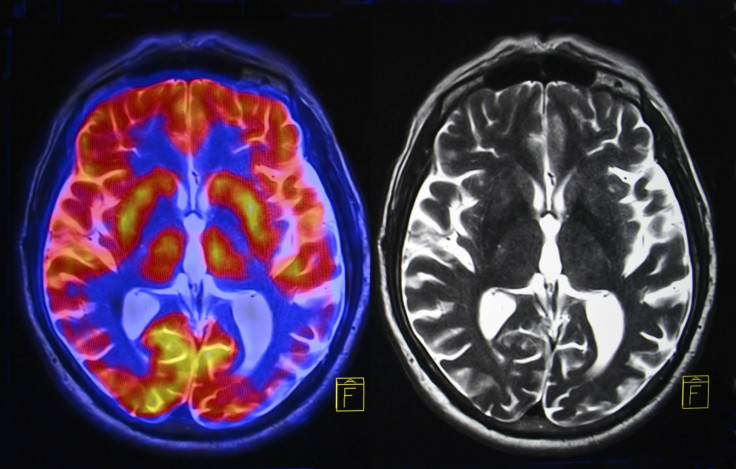
"We knew that HIV could persist in the brain. But what we have identified here are changes to white matter that indicate HIV is replicating in the brain of people whose infection is otherwise under control thanks to ART", Gupta said.
The scans thus offer an opportunity to improve identification of patients with cognitive problems due to HIV-related inflammation – it's a method that is safe and more comfortable for them.
"Where HIV has spread to the brain, we can change the treatment regime to add drugs such as abacavir that cross the blood-brain barrier more effectively to control the infection", Gupta concluded.
© Copyright IBTimes 2025. All rights reserved.





















