HIV 'Breakthrough' Drug Reduces Risk of Infection by up to 92%: What is Truvada?
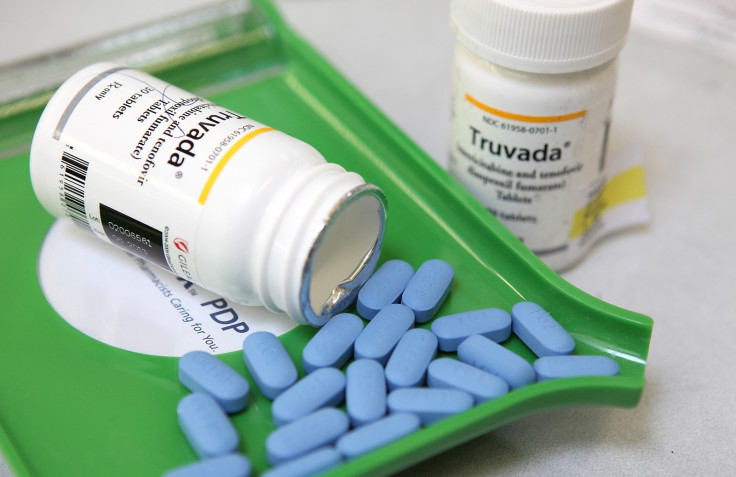
A daily tablet that offers up to a 90% reduction in the risk of contracting HIV could be available in the near future, in what is being hailed as the most significant breakthrough against the virus in a generation.
Truvada provides pre-exposure prophylaxis, a new HIV prevention method for people without the virus, but are at substantial risk of getting it.
The pill contains two medicines, Tenofovir and Emtricitabine, both used in combination with other medicines to treat HIV. When an individual is exposed to the virus through sex or injection drug use, these medicines can work to keep the virus from establishing a permanent infection.
Truvada can be combined with condoms and other prevention methods to provide greater protection, but those taking the drug must visit their GP or doctor for a follow-up every three months.
Dr Sheena McCormack, of the Medical Research Council Clinical Trials Unit at University College London, who is leading a study of the drug, said an interim analysis of data so far showed it could significantly reduce the number of new infections.
"The exciting opportunity this offers is to make the biggest dent in the epidemic of all time. It will be better than treatment as prevention," McCormack told the Independent.
How successful is the drug?
When taken consistently – once a day - Truvada has been shown to reduce the risk of HIV infection in people who are at high risk by up to 92%, according to the Centers for Disease Control and Prevention. It is less effective if it is not taken consistently.
In the UK, an ongoing trial is to be sped up dramatically after it was discovered that taking a single dose of the drug per day provided unprecedented levels of protection against the risk of infection from HIV.
Researchers prescribed Truvada to 407 men taking part in the study in Brighton, London, Manchester, Birmingham, Sheffield and York. Now, another 138 men who had been waiting to trial the medication are going to be offered the drug immediately.
The drug has been approved for use in the United States since 2012. Clinical trials of the drug found that among gay and bisexual men, those taking the drug were 44% less likely overall to get HIV than those given a placebo. Among men with detectable levels of the medicine in their blood, Truvada reduced the risk of infection by up to 92%.
In heterosexually active men and women, Truvada reduced the risk of contracting HIV by 62%. Patients who became infected had far less of the drug in their systems, according to a study published in the New England Journal of Medicine.
In the Partners PrEP Study, funded by a research grant from the Bill & Melinda Gates Foundation, men and women in HIV discordant couples who received the drug were 75% less likely to become infected than those on placebo drugs.
Among injection drug users, the drug reduced the risk of getting HIV by 48%, according to a study of Tenofovir in Bangkok, published in The Lancet.
Are there any side effects?
No significant safety concerns have been detected with the daily use of the medication taken orally. The only reported side effects by some trial participants so far have been upset stomach or loss of appetite, which were mild and usually resolved in the first month.
Researchers have said more studies are needed to determine if and how the drugs affect the sexual behaviour of at-risk individuals.
When will the drug be available on the NHS?
Campaigners have urged the NHS to ensure Truvada is offered to those at risk of infection from HIV as soon as possible. It is hoped the trial can be extended nationally from as early as 2017. The drug could potentially save the NHS millions of pounds each year in long-term treatment.
News of the drug comes amid concerns that the number of gay and bisexual men being diagnosed with HIV reached its highest-ever level in 2013. Following the discovery of Aids in the UK in the early 1980s, there was a steady increase in the number of reported HIV diagnoses, from 8,888 to 15,570, according to the charity Avert.
Yusef Azad, director of policy and campaigns at the National Aids Trust, said: "These encouraging results provide powerful evidence that PrEP should be accessible to all who need it as soon as possible."
© Copyright IBTimes 2025. All rights reserved.





















