Hospital Linked to Child HIV Outbreak Caught Reusing Syringes in Undercover Video After Denying Claims
BBC Eye investigation reveals repeated syringe reuse at THQ Taunsa Hospital that led to a child HIV outbreak despite denials.
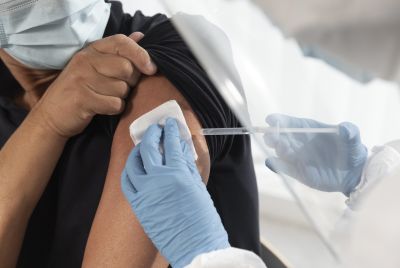
A government facility, THQ Taunsa Hospital in Taunsa, Punjab, Pakistan, has been filmed repeatedly reusing syringes in breach of basic infection control rules, even as senior officials publicly denied that unsafe practices were taking place during a major child HIV outbreak that has affected hundreds of families in the region.
The footage, recorded by BBC Eye in late 2025, comes amid ongoing concern over 331 confirmed child HIV cases in Taunsa between November 2024 and October 2025. Multiple children later tested positive for HIV, including patients with no known alternative source of infection.
For many families, the outbreak is not an abstract public health issue but a personal tragedy. Children previously treated for routine illnesses later became seriously unwell, and in several cases died. One of them, Mohammed Amin, was eight when he died after testing positive. His sister Asma, now 10, was also diagnosed.
The BBC Eye findings suggest a pattern that emerged slowly and then became impossible for local doctors to ignore. A private physician, Dr. Gul Qaisrani, was among the first to raise concerns in late 2024 after noticing a cluster of paediatric HIV cases linked to the same hospital.
He later estimated that dozens of affected children had passed through its wards.
Repeated Syringe Use Captured Despite Infection Control Claims
In the months that followed, provincial authorities promised reforms and suspended senior staff at the hospital. Training programmes were introduced, and officials said infection control would be prioritised. However, BBC undercover filming conducted several months later showed practices that appeared to contradict those assurances.
Across 32 hours of footage, BBC Eye recorded syringes being reused on multi-dose vials on multiple occasions. In several instances, medicine drawn from a vial was then administered to different children, a process that infectious disease specialists say carries a clear risk of contamination.
Dr. Altaf Ahmed, a microbiologist who reviewed the material, said infection could still be transmitted even if needles were changed because contamination can remain in the syringe body itself. His assessment was based on what he observed in the footage rather than any direct examination of patients.
The investigation also documented breaches of hygiene standards. Staff were seen administering injections without sterile gloves, and medical waste was handled without proper protection. In one sequence, a nurse was filmed removing a used syringe from beneath a counter before it was returned into circulation.
Hospital officials have rejected the interpretation of the footage. Dr. Qasim Buzdar, the medical superintendent at the time, said it may have been recorded before his appointment or could have been staged. He insisted the hospital was safe and said infection control training had been implemented across departments.
Official Denials and Leaked Reports
Local government statements have maintained that no definitive epidemiological evidence has established THQ Taunsa as the source of the outbreak. Authorities instead point to wider issues across the healthcare system, including unregulated private clinics and unscreened blood transfusions.
However, a leaked inspection report from a joint mission involving international health organisations described serious concerns in paediatric emergency care, including reused equipment, missing supplies and poor hygiene conditions. It also noted that infection control practices were frequently ignored in high-pressure wards.
Health experts say the problem extends beyond a single facility. Pakistan has one of the highest rates of therapeutic injections globally, many of which are not medically necessary. Combined with supply shortages and weak oversight, this creates conditions in which shortcuts become routine rather than exceptional.
Dr. Fatima Mir of Aga Khan University Hospital said excessive reliance on injections, alongside poor training, increases the risk of transmission when safety protocols break down. She described unsafe injection practices as a 'systemic vulnerability' rather than an isolated failure.
For families in Taunsa, those systemic issues have already translated into personal loss.
© Copyright IBTimes 2025. All rights reserved.